글로벌 연구동향
방사선종양학
- 2023년 03월호
[Cancer Res Treat.] Analysis of Once-Daily Thoracic Radiotherapy Dose According to the Underlying Lung Disease in Patients with Limited-Stage Small Cell Lung Cancer Undergoing Concurrent Chemoradiotherapy
동시항암화학방사선치료를 받은 제한병기 소세포폐암 환자에서 기저폐질환에 따른 방사선량 분석서울의대 / 김병혁, 김학재*
- 출처
- Cancer Res Treat.
- 등재일
- 2023 Jan
- 저널이슈번호
- 55(1):73-82. doi: 10.4143/crt.2021.1202. Epub 2022 Mar 14.
- 내용
-
Abstract
Purpose: In the treatment of concurrent chemoradiotherapy (CCRT) in limited-stage small cell lung cancer, the optimal once-daily radiotherapy (RT) dose/fractionation remain unclear although it is the most frequently used. Therefore, this study aimed to compare the treatment outcomes and toxicities of modest dose RT (≤ 54 Gy) with those of standard dose RT (> 54 Gy) and investigate the benefit of the high dose based on patient factors.Materials and methods: Since 2004, our institution has gradually increased the thoracic RT dose. Among the 225 patients who underwent CCRT, 84 patients (37.3%) received > 54 Gy. Because the patients treated with RT > 54 Gy were not randomly assigned, propensity score matching (PSM) was performed.
Results: The proportion of patients treated with > 54 Gy increased over time (p=0.014). Multivariate analysis revealed that the overall tumor stage and dose > 54 Gy (hazard ratio, 0.65; p=0.029) were independent prognostic factors for overall survival (OS). PSM confirmed that thoracic RT doses of > 54 Gy showed significantly improved progression-free survival (3-year, 42.7% vs. 24.0%; p < 0.001) and OS (3-year, 56.2% vs. 38.5%; p=0.003). Sensitivity analysis also showed that 60 Gy resulted in better survival than 54 Gy. However, in patients with underlying lung disease, OS benefit from > 54 Gy was not observed but considerable rates of severe pulmonary toxicities were observed (p=0.001).
Conclusion: Our analysis supports that the 60 Gy RT dose should be considered in the once-daily regimen of CCRT for limited-stage small cell lung cancer without underlying lung disease, but RT dose > 54 Gy did not seem to benefit for patients with chronic obstructive pulmonary disease or interstitial lung disease. Further study is needed to validate these results.
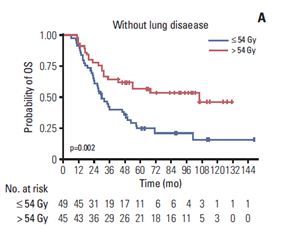
A. 기저 폐질환이 없는 제한병기 소세포폐암 환자들에서 54Gy 이상의 흉부 방사선조사 시 생존율 향상 효과가 있음.
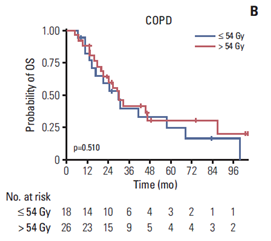
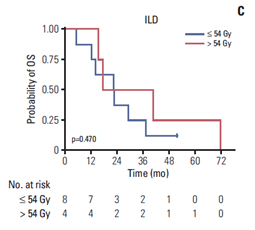
B, C. 폐쇄성 폐질환(B) 과 간질성 폐질환(C)의 기저 질환이 있는 환자들에서는 54Gy 를 기준으로 방사선량에 따른 생존률 차이가 없음.
Affiliations
Byoung Hyuck Kim 1 2, Joo-Hyun Chung 3, Jaeman Son 3, Suzy Kim 1, Hong-Gyun Wu 2 3 4 5, Hak Jae Kim 2 3 4 5
1Department of Radiation Oncology, Seoul Metropolitan Government Seoul National University Boramae Medical Center, Seoul, Korea.
2Department of Radiation Oncology, Seoul National University College of Medicine, Seoul, Korea.
3Department of Radiation Oncology, Seoul National University Hospital, Seoul, Korea.
4Institute of Radiation Medicine, Medical Research Center, Seoul National University, Seoul, Korea.
5Cancer Research Institute, Seoul National University College of Medicine, Seoul, Korea.
- 키워드
- Radiotherapy; Small-cell lung carcinoma; Underlying lung disease.
- 연구소개
- - 소세포폐암은 전체 폐암의 10% 정도를 차지하며, 그 중 완치가 가능한 제한병기의 경우 방사선치료와 항암치료를 동시에 병용하게 된다. 방사선치료 시행에 있어 하루 두 번의 방사선치료가 표준 치료로 권고되고 있지만, 여러 현실적인 문제로 인해 많은 나라에서 하루 한 번의 치료를 시행하고 있는 실정으로 하루 한 번의 치료 시행 시 적정 방사선량에 대해서는 아직도 논란이 있는 상황이다. - 이에 서울대병원과 보라매 병원에서 2004년 이후 제한병기 소세포폐암으로 방사선치료를 시행 받은 225명의 환자들을 대상으로 후향적 분석을 통해 방사선량에 따른 치료 결과를 분석하고, 추가로 폐쇄성 폐질환이나 간질성 폐질환 등 폐에 기저 질환이 있는 환자들에서의 적정 방사선량을 제시하고자 하였다. - 분석 결과 기저 폐질환이 없는 환자들에서는 현재 다수의 가이드라인에서 제시하고 있는 대로 54Gy를 기준으로 그 이상의 선량 특히, 60Gy의 방사선량을 조사 받은 환자들에서 54Gy 이하의 선량을 받은 환자들에 비해 향상된 생존률을 보였지만, 폐쇄성 폐질환이나 간질성 폐질환 등 기저 폐질환이 있는 환자들에서는 조사 선량에 따른 생존률이 차이를 볼 수 없었다. - 본 연구를 통해 현 시대에 제한병기 소세포폐암 환자들에서 60Gy의 방사선치료가 필요함을 재차 확인하였다. 하지만, 폐 기저질환이 있는 환자들은 높은 방사선량을 조사 받을수록 합병증 발생 확률도 높아지기 때문에 그로 인해 치료 이득을 볼 수 없을 가능성을 고려하여, 표준 선량 보다 10% 정도 낮은, 즉 54Gy 정도의 치료 선량을 제시할 수도 있겠다.
- 덧글달기








편집위원
제한적 병기의 소세포폐암에서 기저 폐질환 여부에 따른 dose-response relationship을 보여주는 흥미로운 연구입니다.
덧글달기닫기2023-03-07 08:58:58
등록