글로벌 연구동향
방사선종양학
- [Breast Cancer Res Treat.] Comparison of initial and sequential salvage brain-directed treatment in patients with 1-4 vs. 5-10 brain metastases from breast cancer (KROG 16-12)
서울의대 / 김재식, 김규보, 김인아*
- 출처
- Breast Cancer Res Treat.
- 등재일
- 2023 Jul
- 저널이슈번호
- 200(1):37-45. doi: 10.1007/s10549-023-06936-w.
- 내용
Abstract
Purpose: We aimed to compare the initial and salvage brain-directed treatment and overall survival (OS) between patients with 1-4 brain metastases (BMs) and those with 5-10 from breast cancer (BC). We also organized a decision tree to select the initial whole-brain radiotherapy (WBRT) for these patients.Methods: Between 2008 and 2014, 471 patients were diagnosed with 1-10 BMs. They were divided into two groups based on the number of BM: 1-4 BMs (n = 337) and 5-10 BMs (n = 134). Median follow-up duration was 14.0 months.
Results: Stereotactic radiosurgery (SRS)/fractionated stereotactic radiotherapy (FSRT) was the most common treatment modality (n = 120, 36%) in the 1-4 BMs group. In contrast, 80% (n = 107) of patients with 5-10 BMs were treated with WBRT. The median OS of the entire cohort, 1-4 BMs, and 5-10 BMs was 18.0, 20.9, and 13.9 months, respectively. In the multivariate analysis, the number of BM and WBRT were not associated with OS, whereas triple-negative BC and extracranial metastasis decreased OS. Physicians determined the initial WBRT based on four variables in the following order: number and location of BM, primary tumor control, and performance status. Salvage brain-directed treatment (n = 184), mainly SRS/FSRT (n = 109, 59%), prolonged OS by a median of 14.3 months.
Conclusion: The initial brain-directed treatment differed notably according to the number of BM, which was chosen based on four clinical factors. In patients with ≤ 10 BMs, the number of BM and WBRT did not affect OS. The major salvage brain-directed treatment modality was SRS/FSRT and increased OS.
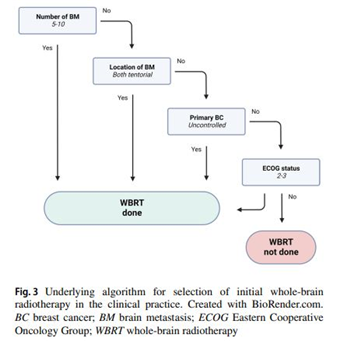
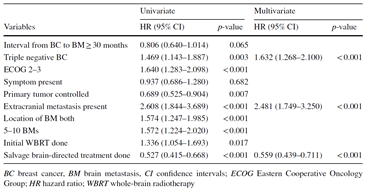
표1. 전체 생존율에 대한 단변량 및 다변량 분석
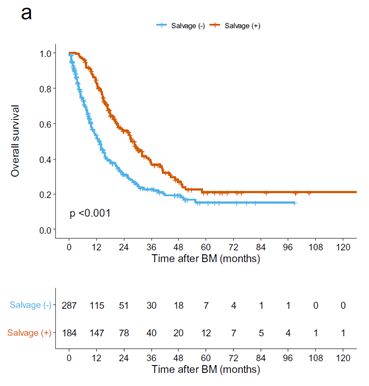
그림 1. Salvage 치료 여부에 따른 전체 생존율 곡선
Affiliations
Jae Sik Kim # 1, Kyubo Kim # 2, Wonguen Jung 2, Kyung Hwan Shin 1, Seock-Ah Im 3, Hee-Jun Kim 4, Yong Bae Kim 5, Jee Suk Chang 5, Jee Hyun Kim 3, Doo Ho Choi 6, Yeon Hee Park 7, Dae Yong Kim 8, Tae Hyun Kim 8, Byung Ock Choi 9, Sea-Won Lee 9 10, Suzy Kim 11, Jeanny Kwon 12, Ki Mun Kang 13, Woong-Ki Chung 14, Kyung Su Kim 1 15, Won Sup Yoon 16, Jin Hee Kim 17, Jihye Cha 18, Yoon Kyeong Oh 19, In Ah Kim 20 21
1Department of Radiation Oncology, Seoul National University College of Medicine, Seoul, Korea.
2Department of Radiation Oncology, Ewha Womans University College of Medicine, Seoul, Korea.
3Department of Internal Medicine, Seoul National University College of Medicine, Seoul, Korea.
4Department of Internal Medicine, Chung-Ang University College of Medicine, Seoul, Korea.
5Department of Radiation Oncology, Yonsei Cancer Center, Yonsei University College of Medicine, Seoul, Korea.
6Department of Radiation Oncology, Samsung Medical Center, Sungkyunkwan University School of Medicine, Seoul, Korea.
7Department of Internal Medicine, Samsung Medical Center, Sungkyunkwan University School of Medicine, Seoul, Korea.
8Proton Therapy Center, National Cancer Center, Seoul, Korea.
9Department of Radiation Oncology, Seoul St. Mary's Hospital, The Catholic University of Korea, Seoul, Korea.
10Department of Radiation Oncology, Eunpyeong St. Mary's Hospital, The Catholic University of Korea, Seoul, Korea.
11Department of Radiation Oncology, Seoul Metropolitan Government Seoul National University Boramae Medical Center, Seoul, Korea.
12Department of Radiation Oncology, Chungnam National University College of Medicine, Daejeon, Korea.
13Department of Radiation Oncology, Gyeongsang National University School of Medicine and Gyeongsang National University Changwon Hospital, Changwon, Korea.
14Department of Radiation Oncology, Chonnam National University Hwasun Hospital, Chonnam National University Medical School, Gwangju, Korea.
15Department of Radiation Oncology, Dongnam Institute of Radiological and Medical Sciences, Busan, Korea.
16Department of Radiation Oncology, Ansan Hospital, Korea University Medical College, Ansan-Si, Korea.
17Department of Radiation Oncology, Keimyung University Dongsan Medical Center, Keimyung University School of Medicine, Daegu, Korea.
18Department of Radiation Oncology, Wonju Severance Christian Hospital, Yonsei University Wonju College of Medicine, Wonju-Si, Korea.
19Department of Radiation Oncology, Chosun University Medical School, Gwangju, Korea.
20Department of Radiation Oncology, Seoul National University College of Medicine, Seoul, Korea. inah228@snu.ac.kr.
21Department of Radiation Oncology, Seoul National University Bundang Hospital, Gumi-Ro 173, 82 Beon-Gil, Bundang Gu, Seongnam, 13620, Republic of Korea. inah228@snu.ac.kr.
#Contributed equally.
- 키워드
- https://pubmed.ncbi.nlm.nih.gov/37138198/
- 연구소개
- 이 연구는 유방암 환자의 뇌전이 수가 1-10개인 경우, 뇌전이 수 (1-4 vs. 5-10)와 초기 전뇌 방사선 치료가 환자의 전체 생존율에 영향을 미치지 않으며, 삼중음성 유방암과 두개 외 전이 여부가 전체 생존율을 감소시킴을 밝혔습니다. 이에 뇌전이 수만을 고려하는 대신 다른 요소들을 종합적으로 고려하여 초기 뇌전이 치료를 선택해야 함을 강조합니다. 또한 salvage 치료로 인한 생존율 이점이 분명하므로, 초기 치료로 정위적 방사선수술 등을 적극적으로 고려하여 환자의 삶의 질을 유지하면서 추후 salvage 치료 가능성을 남겨두어야 합니다. 최종적으로, 이 연구는 10개까지의 뇌전이를 “limited brain metastasis”로 정의할 가능성을 제시하고 있습니다.
- 덧글달기
- 이전글 [Ann Surg .] Importance of Local Ablative Therapies for Lung Metastases in Patients With Colorectal Cancer
- 다음글 [J Gynecol Oncol .] Pattern of practice for postoperative management of endometrial cancer in Korea: a survey by the Korean Gynecologic Oncology Group and the Korean Radiation Oncology Group (KGOG 2028-KROG 2104)










편집위원
유방암의 뇌전이에서 뇌전이 병수 수에 따라 두 군으로 나누어 치료 방법과 예후 등을 분석한 KROG 연구임. 일반적으로 뇌전이 병소 수에 따라 전뇌방사선치료나 정위방사선치료를 선택하게 되는데, 5개 이상의 뇌전이 병소가 있을 경우 정위방사선치료(SRS/FSRT) 보다는 전뇌방사선치료(WBRT)를 선호하는 경향이 있으나, 다변량 분석에서 뇌전이 병소 수 보다는 뇌전이 병소 외(extracranial)의 다른 부위 조절 상태 및 구제요법(salvage) 비율 등이 더 전체생존율에 영향을 미치는 것으로 확인된 점, WBRT가 예후향상에 큰 영향을 끼치지 못했다는 점을 종합해 봤을 때, 10개 이하의 뇌전이 환자에서 뇌전이 병소 수에 따라 WBRT를 우선적으로 결정하지 말고, 뇌전이 병소 외의 다른 부위 조절 상태를 고려해야 한다고 강조하고 있음. 이는 뇌전이 병소 수에 따라 WBRT 여부를 우선적으로 고려하는 일반적인 임상 결정 과정에서 시사하는 바가 큼.
2023-09-06 11:02:10