글로벌 연구동향
방사선종양학
- 2023년 09월호
[Int J Gynecol Cancer .] Radiotherapy in recurrent ovarian cancer: updated results of involved-field radiation therapy
연세의대 / 이병민, 김용배*
- 출처
- Int J Gynecol Cancer .
- 등재일
- 2023 Jul 3
- 저널이슈번호
- 33(7):1106-1111. doi: 10.1136/ijgc-2022-004200.
- 내용
Abstract
Objective: This study aimed to update the possible clinical benefits of radiation therapy in recurrent ovarian cancer.Methods: The medical records of 495 patients with recurrent ovarian cancer after initially undergoing maximal cytoreductive surgery and adjuvant platinum-based chemotherapy based on the pathologic stage between January 2010 and December 2020 were analyzed: 309 and 186 patients were treated without and with involved-field radiation therapy, respectively. Involved-field radiation therapy is defined as radiation therapy only to the areas of the body involved by tumor. The prescribed doses were ≥45 Gy (equivalent dose in 2 Gy/fraction). Overall survival was compared between patients treated with and without involved-field radiation therapy. The favorable group was defined as patients who satisfied at least four of the following factors: good performance, no ascites, normal CA-125, platinum-sensitive tumor, and nodal recurrence.
Results: The median age of the patients was 56 years (range 49-63) and median time to recurrence was 11.1 months (range 6.1-15.5). 217 patients (43.8%) were treated at a single site. Radiation therapy, performance status, CA-125, platinum sensitivity, residual disease, and ascites were all significant prognostic factors. The 3-year overall survival of all patients, patients treated without radiation therapy, and patients treated with radiation therapy was 54.0%, 44.8%, and 69.3%, respectively. Radiation therapy was associated with higher overall survival rates in the unfavorable and favorable patient groups. Patient characteristics showed higher rates of normal CA-125, lymph node metastasis only, lower platinum sensitivity, and higher rates of ascites in the radiation therapy group. After propensity score matching, the radiation therapy group showed superior overall survival to the non-radiation therapy group. Normal CA-125, good performance status, and platinum sensitivity were associated with a good prognosis in patients treated with radiation therapy.
Conclusion: Our study showed that higher overall survival was observed in patients treated with radiation therapy in recurrent ovarian cancer.
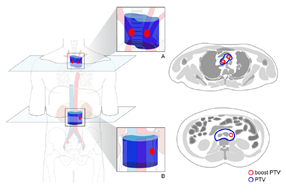
그림 1. 방사선치료의 예시
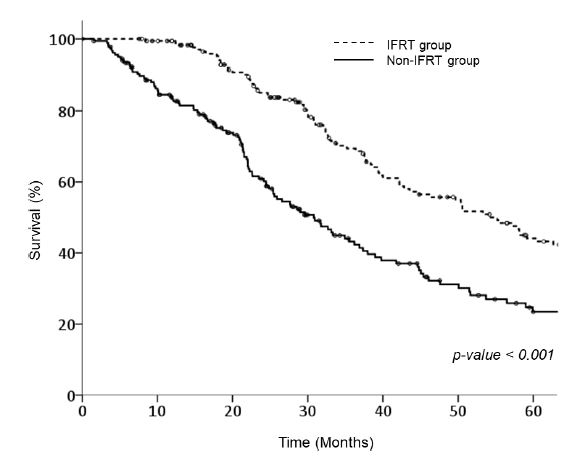
그 림 2. Propensity score matching 이후 두 군 간의 overall survival 비교
Affiliations
Byung Min Lee 1 2, Seo Jin Lee 2, Nalee Kim 3, Hwa Kyung Byun 2, Yong Bae Kim 4
1Radiation Oncology, Uijeongbu St Mary's Hospital, Seoul, Korea (the Republic of).
2Department of Radiation Oncology, Yonsei University College of Medicine, Seodaemun-gu, Korea (the Republic of).
3Radiation Oncology, Samsung Seoul Hospital, Gangnam-gu, Seoul, Korea (the Republic of).
4Department of Radiation Oncology, Yonsei University College of Medicine, Seodaemun-gu, Korea (the Republic of) ybkim3@yuhs.ac.
- 키워드
- Ovarian Cancer; Radiotherapy.
- 연구소개
- 난소암은 대부분 진행된 후 진단이 되어 표준 치료를 받은 후 재발율이 80%에 달하며, 재발 시 10년 무병생존율이 15% 미만으로, 부인암 중 예후가 가장 불량합니다. 본 연구는 종양감축술 및 보조적 항암화학요법 후 재발한 난소암 환자에서 involved field radiotherapy (IFRT)의 치료 성적에 관한 연구입니다. 총 495명의 재발성 난소암 환자 중 IFRT를 받은 환자가 186명, IFRT를 시행 받지 않은 환자가 309명이었으며, 두 환자군의 3년 생존율을 비교하였을 시 IFRT를 시행 받은 군은 69.3%, IFRT를 시행 받지 않은 군은 44.8%로 두 군 간 유의한 생존율 차이를 보였습니다. 이러한 생존율 차이는 두 군 간 환자 특성을 propensity score matching 한 이후에도 유지되었습니다. 또한 다변량분석시 전신수행상태가 좋고, CA-125가 정상범위이며, platinum-sensitive한 종양, 수술 후 잔여 종양이 없었던 경우, 복수가 없는 경우, IFRT를 시행한 경우가 우수한 생존율과 연관된 인자로 나타났습니다. 본 연구는 재발성 난소암에서 방사선치료가 생존율을 향상시킬 수 있음을 보여주었다는 점에서 의미가 있는 연구라 생각됩니다. 이 결과를 바탕으로 현재 암정복추진연구개발사업의 지원을 받아 “재발성 난소암의 표준구제 치료요법에 정위체부방사선치료 추가효과에 대한 전향적 제3상 다기관 임상연구 (SABR-ROC, KGOG3064/KROG2204)”를 수행중이며 국제 다기관연구로 확대하고 있습니다
- 덧글달기
- 이전글 [J Gynecol Oncol .] Pattern of practice for postoperative management of endometrial cancer in Korea: a survey by the Korean Gynecologic Oncology Group and the Korean Radiation Oncology Group (KGOG 2028-KROG 2104)
- 다음글 [J Cancer Res Clin Oncol .] Novel scoring system guiding the incorporation of adjuvant RT for neuroendocrine neoplasms treated with surgical resection followed by chemotherapy







