글로벌 연구동향
방사선종양학
- 2022년 06월호
[Cancer Res Treat.] Effect of Postoperative Radiotherapy after Primary Tumor Resection in De Novo Stage IV Breast Cancer: A Multicenter Retrospective Study (KROG 19-02) 4기 유방암에서 원발종양 절제와 수술후 방사선치료 효과에 대한 다기관연구 (KROG 19-02)서울의대, 울산의대 / 김연주, 신경환*, 김수산*
- 출처
- Cancer Res Treat.
- 등재일
- 2022 Apr
- 저널이슈번호
- 54(2):478-487. doi: 10.4143/crt.2021.632.
- 내용
-
Abstract
Purpose: This study aimed to investigate the impact of postoperative radiotherapy (PORT) in de novo metastatic breast cancer (dnMBC) patients undergoing planned primary tumor resection (PTR) and to identify the subgroup of patients who would most benefit from PORT.Materials and methods: This study enrolled 426 patients with dnMBC administered PTR alone or with PORT. The primary and secondary outcomes were overall and progression-free survival (OS and PFS), respectively.
Results: The median follow-up time was 53.7 months (range, 3.1 to 194.4). The 5-year OS and PFS rates were 73.2% and 32.0%, respectively. For OS, clinical T3/4 category, triple-negative breast cancer (TNBC), postoperative chemotherapy alone were significantly poor prognostic factors, and administration of PORT failed to show its significance. Regarding PFS, PORT was a favorable prognostic factor (hazard ratio, 0.64; 95% confidence interval, 0.50 to 0.82; p < 0.001), in addition to T1/2 category, ≤ 5 metastases, and non-TNBC. According to the multivariate analyses of OS in the PORT group, we divided the patients into three groups (group 1, T1/2 and non-TNBC [n=193]; group 2, T3/4 and non-TNBC [n=171]; and group 3, TNBC [n=49]), and evaluated the effect of PORT. Although PORT had no significance for OS in all subgroups, it was a significant factor for good prognosis regarding PFS in groups 1 and 2, not in group 3.
Conclusion: PORT was associated with a significantly better PFS in patients with dnMBC who underwent PTR. Patients with clinical T1/2 category and non-TNBC benefited most from PORT, while those with TNBC showed little benefit.
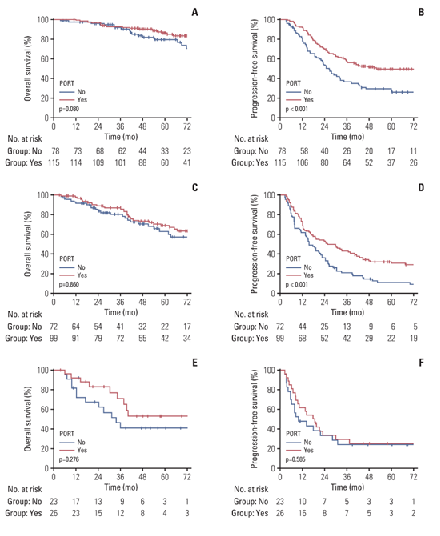
환자들을 크게 group 1 [T1/2 and non-triple negative breast cancer (TNBC), 그림 A와 B], group 2 (T3/4 and non-TNBC, 그림 C와 D), 그리고 group 3 (TNBC, 그림 E와 F)로 나누어서 분석했을 때, 비록 술후 방사선치료가 전체 생존율에서는 의미 있는 인자가 아니었지만, 무진행생존율에 대해서는 통상 가장 예후가 나쁜 TNBC군을 제외하고는 술후 방사선치료가 의미 있는 인자로 밝혀졌습니다.
Affiliations
Yeon Joo Kim 1 , Yeon-Joo Kim 2 , Yong Bae Kim 3 , Ik Jae Lee 4 , Jeanny Kwon 5 , Kyubo Kim 6 , Jihye Cha 7 , Myungsoo Kim 8 , In Young Jo 9 , Jung Hoon Kim 10 , Jaehyeon Park 11 , Jin Hee Kim 12 , Juree Kim 13 , Kyung Hwan Shin 14 , Su Ssan Kim 1
1 Department of Radiation Oncology, Asan Medical Center, University of Ulsan College of Medicine, Seoul, Korea.
2 Proton Therapy Center, National Cancer Center, Goyang, Korea.
3 Department of Radiation Oncology, Yonsei Cancer Center, Yonsei University College of Medicine, Seoul, Korea.
4 Department of Radiation Oncology, Gangnam Severance Hospital, Yonsei University College of Medicine, Seoul, Korea.
5 Department of Radiation Oncology, Chungnam National University College of Medicine, Daejeon, Korea.
6 Department of Radiation Oncology, Ewha Womans University College of Medicine, Seoul, Korea.
7 Department of Radiation Oncology, Wonju Severance Christian Hospital, Yonsei University Wonju College of Medicine, Wonju, Korea.
8 Department of Radiation Oncology, Incheon St. Mary's Hospital, College of Medicine, The Catholic University of Korea, Incheon, Korea.
9 Department of Radiation Oncology, Soonchunhyang University Hospital, Cheonan, Korea.
10 Department of Radiation Oncology, Konyang University College of Medicine, Daejeon, Korea.
11 Department of Radiation Oncology, Yeungnam University Medical Center, Yeungnam University College of Medicine, Daegu, Korea.
12 Department of Radiation Oncology, Dongsan Medical Center, Keimyung University School of Medicine, Daegu, Korea.
13 Department of Radiation Oncology, CHA Ilsan Medical Center, CHA University School of Medicine, Goyang, Korea.
14 Department of Radiation Oncology, Seoul National University College of Medicine, Seoul, Korea.
- 키워드
- Breast surgery; Postoperative radiotherapy; Stage IV breast cancer; Survival.
- 연구소개
- 진단 당시 4기 유방암인 환자들에서 원발 유방 종양에 대해서 절제술을 시행한 경우 술후 방사선치료의 효과에 대해 분석하고, 어떤 환자군에서 술후 방사선치료가 가장 도움이 되는지 또한 알아보고자 하였습니다.
- 덧글달기








편집위원
4기 유방암에서 국소치료의 역할에 대한 논란이 여전한 가운데, 수술 후 방사선치료의 역할에 대해 국내 다기관의 자료를 후향적으로 분석한 연구로, 전체 생존율에는 영향이 없었으나 무진행 생존율에서 이득이 있는 그룹을 제시한 논문
덧글달기닫기2022-06-08 14:35:32
등록
편집위원2
진단시 병기4기인 경우 원발병소의 수술과 방사선치료가 생존율에 미치는 영향을 다기관으로 분석한 연구로 국소치료가 도움이 되는 하위집단을 제시했다는 면에서 의의가 있습니다.
덧글달기닫기2022-06-09 15:41:23
등록