글로벌 연구동향
방사선종양학
- 2022년 02월호
[Breast.] Novel prognostic classification predicts overall survival of patients receiving salvage whole-brain radiotherapy for recurrent brain metastasis from breast cancer: A recursive partitioning analysis (KROG 16-12)서울의대 / 김재식, 김규보, 김인아*
- 출처
- Breast.
- 등재일
- 2021 Dec
- 저널이슈번호
- 60:272-278. doi: 10.1016/j.breast.2021.11.005. Epub 2021 Nov 15.
- 내용
Abstract
Background: To investigate outcomes of salvage whole-brain radiotherapy (WBRT) for recurrent brain metastases (BM) from breast cancer (BC), to identify prognostic factors of overall survival (OS), and to propose a novel prognostic classification for OS in these patients.Materials and methods: We identified 54 patients who had received salvage WBRT as the second brain-focused treatment for recurrent BM from BC (2000-2014). The median follow-up duration was 4.9 months. A recursive partitioning analysis (RPA) was conducted to develop a model to predict OS at the time of salvage WBRT.
Results: The median OS was 6.8 months. OS according to BC-specific graded prognostic assessment (breast-GPA), modified breast-GPA, and updated breast-GPA did not represent our cohort. In the multivariate analysis, a long time before salvage WBRT (≥16 months), control of primary BC or extracranial metastases, systemic treatment after salvage WBRT, and administration of a biologically effective dose for an α/β of 10 Gy (BED10) of salvage WBRT >37.5 Gy showed superior OS. We proposed three RPA classes based on the control of both primary BC and extracranial metastasis and BED10 of salvage WBRT: class I, class II, and class III. In this model, patients with class I experienced the best OS (34.6 months; class II, 5.0 months; class III, 2.4 months; P < 0.001).
Conclusions: In our RPA classification according to the control of both primary BC and extracranial metastasis and the dose of salvage WBRT, significant differences in OS were observed. The subsequent use of a systemic treatment showed better OS.
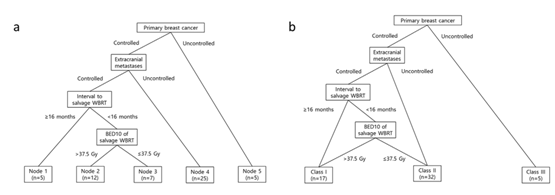
Fig 1. Diagrams of recursive partitioning analysis (RPA). (a) Five terminal nodes before amalgamation. (b) Final three RPA classes after amalgamation.
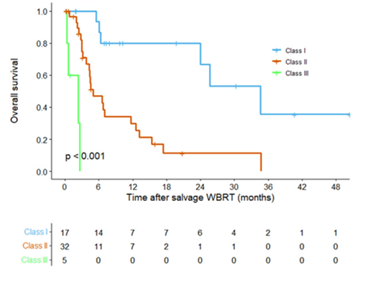
Fig 2. Overall survival according to the novel recursive partitioning analysis class.
Affiliations
Jae Sik Kim 1 , Kyubo Kim 2 , Wonguen Jung 2 , Kyung Hwan Shin 1 , Seock-Ah Im 3 , Yong Bae Kim 4 , Jee Suk Chang 4 , Doo Ho Choi 5 , Haeyoung Kim 5 , Yeon Hee Park 6 , Dae Yong Kim 7 , Tae Hyun Kim 7 , Jeanny Kwon 8 , Ki Mun Kang 9 , Woong-Ki Chung 10 , Kyung Su Kim 11 , In Ah Kim 12
1 Department of Radiation Oncology, Seoul National University College of Medicine, South Korea.
2 Department of Radiation Oncology, Ewha Womans University College of Medicine, South Korea.
3 Department of Internal Medicine, Seoul National University College of Medicine, South Korea.
4 Department of Radiation Oncology, Yonsei Cancer Center, Yonsei University College of Medicine, South Korea.
5 Department of Radiation Oncology, Samsung Medical Center, Sungkyunkwan University School of Medicine, South Korea.
6 Department of Internal Medicine, Samsung Medical Center, Sungkyunkwan University School of Medicine, South Korea.
7 Proton Therapy Center, National Cancer Center, South Korea.
8 Department of Radiation Oncology, Chungnam National University College of Medicine, South Korea.
9 Department of Radiation Oncology, Gyeongsang National University School of Medicine and Gyeongsang National University Changwon Hospital, South Korea.
10 Department of Radiation Oncology, Chonnam National University Hwasun Hospital, Chonnam National University Medical School, South Korea.
11 Department of Radiation Oncology, Dongnam Institute of Radiological and Medical Sciences, South Korea; Department of Radiation Oncology, Ewha Womans University College of Medicine, South Korea.
12 Department of Radiation Oncology, Seoul National University College of Medicine, South Korea; Department of Radiation Oncology, Seoul National University Bundang Hospital, South Korea. Electronic address: inah228@snu.ac.kr.
- 키워드
- Brain metastasis; Breast cancer; Overall survival; Recursive partitioning analysis; Whole-brain radiotherapy.
- 연구소개
- 유방암 환자에서 뇌전이가 증가하고 있으며, 여러 권고안에서 limited disease에서는 whole-brain radiotherapy (WBRT) 대신에 stereotactic radiosurgery를 시행할 것을 권고하고 있어, 재발성 뇌전이에 대한 재치료가 증가할 것으로 예상됩니다. 그러나 뇌전이 재발 이후 시행되는 salvage WBRT에 대해서는 많이 알려진 바가 없습니다. 본 연구에서 salvage WBRT를 받은 경우 median overall survival (OS)은 6.8개월이었으며, 여러 graded prognostic assessment (GPA)와 OS와의 관련성은 크지 않았습니다. 이는 GPA system이 초기 뇌전이 환자를 바탕으로 만들어져 뇌전이 재발의 경우를 잘 반영하지 못한 결과로 생각됩니다. 이에 본 연구에서 처음으로 salvage WBRT를 받는 환자에서 새로운 recursive partitioning analysis classification을 제시하며 (Fig 1), OS를 잘 반영함을 확인하였습니다 (Fig 2).
- 덧글달기
- 이전글 [Radiother Oncol.] Extended application of a CT-based artificial intelligence prognostication model in patients with primary lung cancer undergoing stereotactic ablative radiotherapy
- 다음글 [Mutat Res Genet Toxicol Environ Mutagen.] Chromosome aberration dynamics in breast cancer patients treated with radiotherapy: Implications for radiation biodosimetry








편집위원
유방암 뇌전이로 구제 목적의 전뇌방사선치료를 받은 환자의 예후인자를 분석하였고, 원발종양과 두개외 전이종양의 조절상태 및 구제 전뇌방사선치료선량, 그리고 방사선치료 후 전신치료가 생존율에 유의한 인자로 분석됨
덧글달기닫기2022-01-14 15:40:14
등록