글로벌 연구동향
방사선종양학
- 2022년 01월호
[Technol Cancer Res Treat.] Clinical Outcome of Salvage Radiotherapy for Locoregional Clinical Recurrence After Radical Prostatectomy국립암센터 / 이성욱, 조관호*
- 출처
- Technol Cancer Res Treat.
- 등재일
- Jan-Dec 2021
- 저널이슈번호
- 20:15330338211041212. doi: 10.1177/15330338211041212.
- 내용
Abstract
Objectives: To assess the clinical outcomes of prostate cancer patients treated with salvage radiotherapy (SRT) for locoregional clinical recurrence (CR) after radical prostatectomy (RP). Methods: Records of 60 patients with macroscopic locoregional recurrence after prostatectomy and referrals for SRT were retrospectively investigated in the multi-institutional database. The median radiation dose was 70.2 Gy. Biochemical failure was defined as the prostate-specific antigen (PSA) ≥ nadir + 2 or initiation of androgen deprivation therapy (ADT) for increased PSA. Results: Median recurrent tumor size was 1.1 cm and pre-radiotherapy PSA level was 0.4 ng/ml. At a median follow-up of 83.1-month after SRT, 7-year biochemical failure-free survival (BCFFS), locoregional failure-free survival (LRFFS), distant metastasis-free survival (DMFS), and overall survival (OS) were 67.0%, 89.7%, 83.6%, and 91.2%, respectively. Higher Gleason's scores were associated with unfavorable BCFFS, DMFS, and OS. Pre-SRT PSA ≥0.5 ng/ml predicted worse BCFFS, LRFFS, and DMFS. In multivariate analyses, a Gleason's score of 8 to 10 was associated with decreased BCFFS (hazard ratio [HR] 3.12, 95% confidence interval [CI] 1.11-8.74, P = .031) and OS (HR 17.72, 95% CI 1.75-179.64, P = .015), and combined ADT decreased the risks of distant metastasis (HR 0.18, 95% CI 0.04-0.92, P = .039). Two patients (3.3%) experienced late grade 3 urinary toxicity. Conclusions: SRT for locoregional CR after RP achieved favorable outcomes with acceptable long-term toxicities. Higher Gleason's scores and pre-radiotherapy PSA level were unfavorable prognostic variables. Combined ADT may decrease the risks of metastases.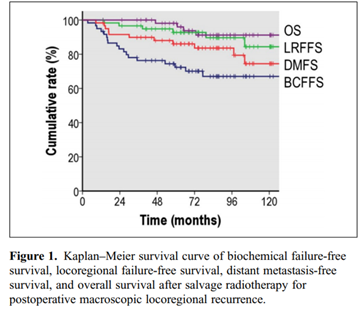
Affiliations
Sung Uk Lee 1 , Kwan Ho Cho 1 , Jin Ho Kim 2 , Young Seok Kim 3 , Taek-Keun Nam 4 , Jae-Sung Kim 5 , Jaeho Cho 6 , Seo Hee Choi 6 , Su Jung Shim 7 , Jin Hee Kim 8 , Ah Ram Chang 9
1 The Proton Therapy Center, Research Institute and Hospital70317National Cancer Center, Goyang, Korea.
2 65462Department of Radiation Oncology, Seoul National University Hospital, 37990Seoul National University College of Medicine, Seoul, Korea.
3 Department of Radiation Oncology, Asan Medical Center, 35029University of Ulsan College of Medicine, Seoul, Korea.
4 65722Department of Radiation Oncology, Chonnam National University Hwasun Hospital, Chonnam National University College of Medicine, Hwasun, Korea.
5 Department of Radiation Oncology, Yonsei Cancer Center, 37991Yonsei University College of Medicine, Seoul, Korea.
6 46666Department of Radiation Oncology, Eulji Hospital, Eulji University School of Medicine, Seoul, Korea.
7 Dongsan Medical Center, 65673Keimyung University School of Medicine, Daegu, Korea.
8 Department of Radiation Oncology, Dongsan Medical Center, Keimyung University School of Medicine, Daegu, Korea.
9 71544Department of Radiation Oncology, Soonchunhyang University Hospital, Seoul, Korea.
1 The Proton Therapy Center, Research Institute and Hospital70317National Cancer Center, Goyang, Korea.
2 65462Department of Radiation Oncology, Seoul National University Hospital, 37990Seoul National University College of Medicine, Seoul, Korea.
3 Department of Radiation Oncology, Asan Medical Center, 35029University of Ulsan College of Medicine, Seoul, Korea.
4 65722Department of Radiation Oncology, Chonnam National University Hwasun Hospital, Chonnam National University College of Medicine, Hwasun, Korea.
5 Department of Radiation Oncology, Yonsei Cancer Center, 37991Yonsei University College of Medicine, Seoul, Korea.
6 46666Department of Radiation Oncology, Eulji Hospital, Eulji University School of Medicine, Seoul, Korea.
7 Dongsan Medical Center, 65673Keimyung University School of Medicine, Daegu, Korea.
8 Department of Radiation Oncology, Dongsan Medical Center, Keimyung University School of Medicine, Daegu, Korea.
9 71544Department of Radiation Oncology, Soonchunhyang University Hospital, Seoul, Korea.
- 키워드
- prostatectomy; prostatic neoplasms; radiotherapy; recurrence.
- 연구소개
- 전립선암의 근치적 수술 후 국소재발한 환자에서 salvage radiotherapy의 효과를 분석한 연구입니다. 전립선암에서는 biochemical recurrence라고 불리는 PSA 상승이 흔히 국소재발보다 선행합니다. 그렇기 때문에 salvage radiotherapy는 주로 biochemical recurrence에 대하여 시행되어, 국소재발한 환자에 대한 salvage radiotherapy를 시행하는 경우는 임상적으로 드문 상황입니다. 이에 다기관 후향적 연구로 60명의 환자를 포함하여 분석하였습니다. 이 환자들에 대한 salvage radiotherapy 후 7년 국소제어율 및 생존율이 각각 89.7% 및 91.2%로 우수하게 보고되었습니다. 예후 인자로는 Gleason’s score와 호르몬 치료의 병합 여부가 파악되었습니다. 전립선암 환자를 진료보시는 임상의들에게 소개 및 도움이 될 만한 좋은 정보라 생각합니다.
- 덧글달기







