글로벌 연구동향
방사선종양학
- [Radiother Oncol .] Adjuvant radiotherapy in node-negative salivary malignancies of the parotid gland: A multi-institutional analysis
연세의대 / 박정빈, 위찬우*
- 출처
- Radiother Oncol .
- 등재일
- 2023 Jun
- 저널이슈번호
- 183:109554. doi: 10.1016/j.radonc.2023.109554.
- 내용
Abstract
Background and purpose: To determine the role of adjuvant radiotherapy (ART) in parotid gland cancer without nodal metastasis, we evaluated the survival outcomes, prognostic factors, and dose-response relationships in patients with node-negative parotid gland cancer patients.Materials and methods: Patients who underwent curative parotidectomy and were pathologically diagnosed with parotid gland cancer without regional or distant metastases between 2004 and 2019 were reviewed. The benefit of ART in terms of locoregional control (LRC) and progression-free survival (PFS) were evaluated.
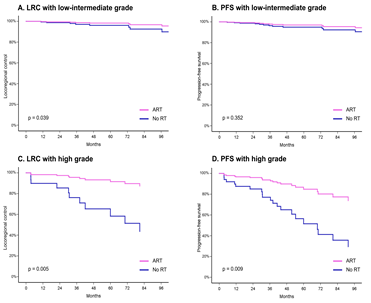
Results: In total, 261 patients were included in the analysis. Of them, 45.2 % received ART. The median follow-up period was 66.8 months. Multivariate analysis revealed that histological grade and ART were independent prognostic factors for LRC and PFS (all p <.05). For patients with high-grade histology, ART was associated with a significant improvement in 5-year LRC (p =.005) and PFS (p =.009). Among patients with high-grade histology who completed RT, higher biologic effective dose (≥77 Gy10) significantly increased PFS (adjusted hazard ratio [HR], 0.10 per 1-Gy increase; 95 % confidence interval [CI], 0.02-0.58; p =.010). ART significantly improved LRC (p =.039) in patients with low-to-intermediate histological grade as well per multivariate analysis, and subgroup analyses revealed patients with T3-4 stage and close/positive resection margins (<1 mm) would benefit from ART.
Conclusion: ART should be strongly recommended for patients with node-negative parotid gland cancer with high-grade histology in terms of disease control and survival. In patients with low-to-intermediate-grade disease, those with high T stage and incomplete resection margin benefit with ART.
Affiliations
Jung Bin Park 1, Hong-Gyun Wu 2, Jin Ho Kim 2, Joo Ho Lee 2, Soon-Hyun Ahn 3, Eun-Jae Chung 3, Keun-Yong Eom 4, Woo-Jin Jeong 5, Tack-Kyun Kwon 6, Suzy Kim 7, Chan Woo Wee 8
1Department of Radiation Oncology, Seoul National University Hospital, Seoul National University College of Medicine, Seoul, Republic of Korea. Electronic address: pjbin9314@gmail.com.
2Department of Radiation Oncology, Seoul National University Hospital, Seoul National University College of Medicine, Seoul, Republic of Korea.
3Department of Otorhinolaryngology-Head and Neck Surgery, Seoul National University Hospital, Seoul National University College of Medicine, Seoul, Republic of Korea.
4Department of Radiation Oncology, Seoul National University Bundang Hospital, Seoul National University College of Medicine, Seongnam, Republic of Korea.
5Department of Otorhinolaryngology-Head and Neck Surgery, Seoul National University Bundang Hospital, Seoul National University College of Medicine, Seongnam, Republic of Korea.
6Department of Otorhinolaryngology-Head and Neck Surgery, SMG-SNU Boramae Medical Center, Seoul National University College of Medicine, Seoul, Republic of Korea.
7Department of Radiation Oncology, SMG-SNU Boramae Medical Center, Seoul National University College of Medicine, Seoul, Republic of Korea.
8Department of Radiation Oncology, SMG-SNU Boramae Medical Center, Seoul National University College of Medicine, Seoul, Republic of Korea. Electronic address: wcw0108@hanmail.net.
- 키워드
- Histological grade; Parotid gland cancer; Radiation; Radiotherapy; Salivary gland cancer.
- 연구소개
- - 연구과제 수행 중 생긴 에피소드: 이하선암이 다양한 조직형과 특성을 갖고 있다보니 환자군을 모은 후 이질성을 어떻게 정리해야 할지 많은 고민이 있었습니다. 그리고 유의미한 결과를 찾아낼 수 있는 분석 방법을 정하기 위해 여러 시도를 했었습니다. - 연구과제 수행 중 보람되었던 일: 침샘암은 조직학적 아형이 다양하고 환자 수가 많지 않아 전향적 무작위 임상연구가 이루어지기 쉽지 않은데, 다기관 후향적 연구를 통해 방사선치료의 효용성과 선량-반응 효과를 파악할 수 있었습니다. - 이 분야로 진학하려는 후배들을 위한 조언: 방사선치료 기술의 발전으로 암환자의 생존율 및 국소제어율에 아주 핵심적인 역할을 하고 있지만 여러 암종에서 방사선치료의 효과 및 적정 선량에 대해서는 아직도 연구해야 할 주제들이 많습니다. 발생률이 낮은 암종에서는 대규모 전향적 무작위 연구를 진행하기 어려운 면이 있기에, 여러 기관의 선생님들과 협력하여 다기관 임상 연구를 수행하는 것이 이런 경우에 도움이 될거 같습니다. - 연구활동 관련 계획: 방사선치료로 인한 독성은 두경부암 환자들의 삶의 질에 큰 영향을 미칩니다. 방사선치료의 효과와 독성 사이에서 적정 선량을 밝혀내고 이를 통해 환자들에게 가장 도움이 될 수 있는 치료를 시행하는 것이 중요합니다. 이하선암 뿐 아니라 다른 암종에서도 방사선치료를 필요로 하는 risk factor나 선량을 정의할 수 있는 연구를 진행할 예정입니다.
- 덧글달기
- 이전글 [Asia Pac J Clin Oncol .] Consolidative high-dose thoracic radiotherapy for limited metastatic nonsmall cell lung cancer: Focusing on oligo-progressive disease
- 다음글 [Radiother Oncol .] Prognosis prediction for glioblastoma multiforme patients using machine learning approaches: Development of the clinically applicable model










편집위원
임파절 전이가 없는 침샘암에서 수술후 방사선치료(ART)의 효용성을 분석한 다기관 임상연구임. 다변량 분석에서 조직등급(histological grade)과 ART 여부가 예후 인자로 확인되었으며, 고등급(high-grade) 침샘암, 저-중등급에서 T3-4 병기 및 불완전한 종양 절연면(close/positive resection margin)일 경우 ART가 예후에 긍정적인 도움을 줄 수 있으므로 ART를 강력하게 추천한다는 결론을 도출함. 이를 통해 실제 임상에서 임파절 전이가 없는 침샘암 환자의 보조적 방사선치료 여부를 결정할 수 있는 근거로 삼을 수 있을 것으로 기대됨.
2023-08-08 14:02:11