글로벌 연구동향
방사선종양학
- 2021년 05월호
[Gynecol Oncol.] Magnetic resonance imaging-based validation of the 2018 FIGO staging system in patients treated with definitive radiotherapy for locally advanced cervix cancer연세의대 / 김진아, 김준원*
- 출처
- Gynecol Oncol.
- 등재일
- 2021 Mar
- 저널이슈번호
- 160(3):735-741. doi: 10.1016/j.ygyno.2020.12.012. Epub 2020 Dec 22.
- 내용
Abstract
Objective: To validate the revised 2018 International Federation of Gynecologic and Obstetrics (FIGO) staging system in patients who underwent diagnostic magnetic resonance imaging (MRI) and radiotherapy (RT) for locally advanced cervix cancer.Methods: We analyzed 677 patients who were diagnosed with pelvic MRI and treated with definitive (chemo-)RT for locally advanced cervix cancer (stage IB2/IIA2-IVA or N+) between 1992 and 2018. Patients were classified according to 2009 and 2018 FIGO staging, and survival outcomes were compared. We developed a nomogram to improve prediction of progression-free survival (PFS).
Results: Pelvic and paraaortic lymph nodes were positive in 331 (48.9%) and 78 (11.5%) patients, respectively. At a median follow-up of 77.9 months, the 5-year PFS was 83.5%, 65.2%, 71.0%, 60.6%, 37.6% and 38.9% for IB, IIA, IIB, IIIA, IIIB and IVA according to FIGO 2009 and 88.9%, 60.0%, 73.8%, 66.7%, 36.3%, 68.9%, 43.6%, and 38.9% for IB, IIA, IIB, IIIA, IIIB, IIIC1, IIIC2, and IVA according to FIGO 2018, respectively. Survival of stage IIIC cervix cancer depended on the local extent of the tumor: the 5-year PFS of T1, T2, and T3 stages were 80.3%, 73.9%, and 45.5% for IIIC1 and 100%, 44.9%, and 23.4% for IIIC2. Histology, tumor size, node metastasis, FIGO 2009, and treatment modality were independent prognostic factors in the Cox regression analysis, and the nomogram incorporating these factors outperformed FIGO 2009 and FIGO 2018 (AUC 0.718 vs. 0.616 vs. 0.594).
Conclusions: FIGO 2018 revision was associated with heterogenous outcomes among stage III cervix cancer patients. Our nomogram can assist the FIGO system in predicting PFS after definitive RT.
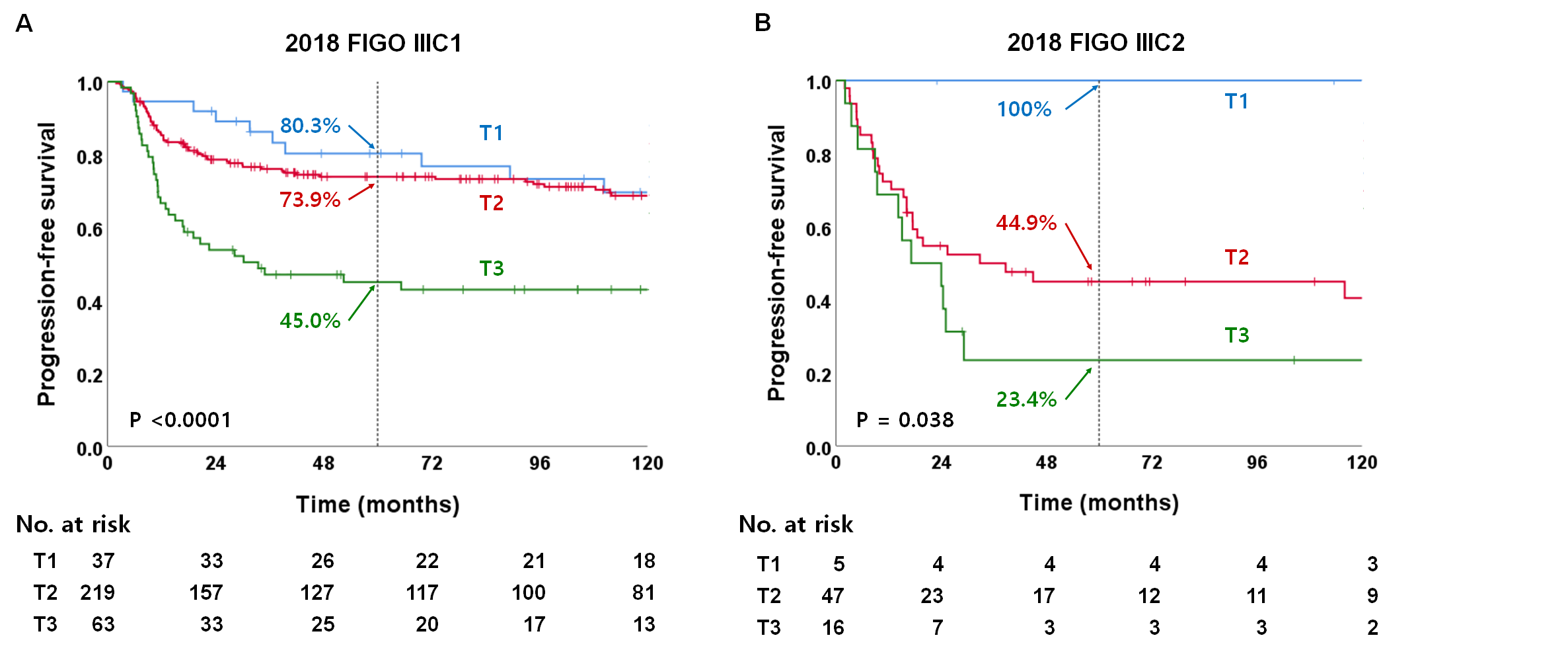
Figure 2. 2018 FIGO 병기에 새로 추가된 IIIC1과 IIIC2 환자에서 T1 병기에 따른 무진행 생존율 비교
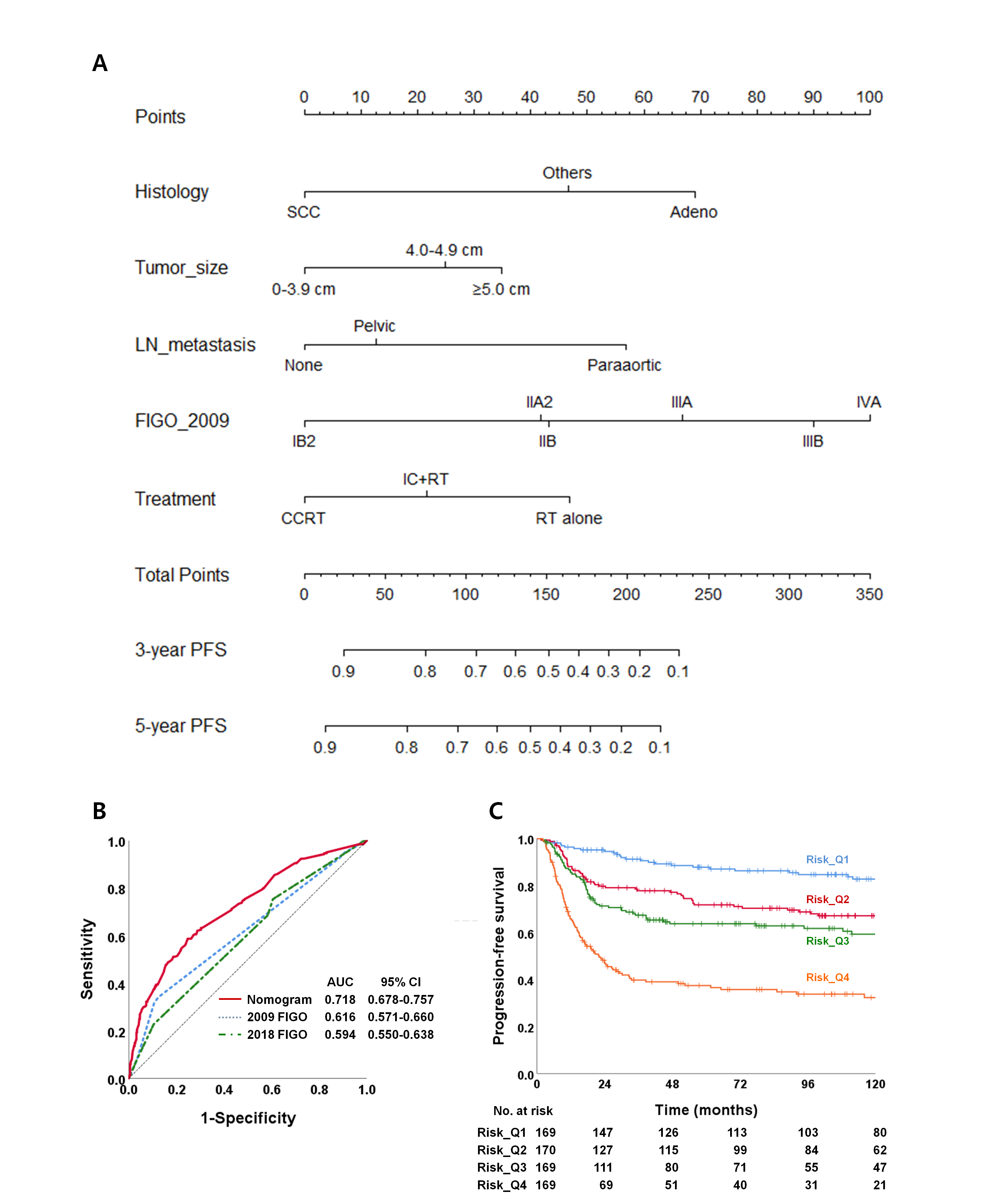
Figure 3. 2009년 FIGO 병기와 기타 예후 인자들을 반영한 노모그램의 무진행 생존율 예측
Affiliations
Jina Kim 1 , Yeona Cho 2 , Nalee Kim 3 , Seung Yeun Chung 4 , Jun Won Kim 5 , Ik Jae Lee 2 , Yong Bae Kim 1
1 Department of Radiation Oncology, Yonsei Cancer Center, Yonsei University College of Medicine, Seoul, Republic of Korea.
2 Department of Radiation Oncology, Gangnam Severance Hospital, Yonsei University College of Medicine, Seoul, Republic of Korea.
3 Department of Radiation Oncology, Samsung Medical Center, Sungkyunkwan University School of Medicine, Seoul, Republic of Korea.
4 Department of Radiation Oncology, Ajou University Hospital, Ajou University School of Medicine, Suwon, Republic of Korea.
5 Department of Radiation Oncology, Gangnam Severance Hospital, Yonsei University College of Medicine, Seoul, Republic of Korea. Electronic address: junwon@yuhs.ac.
- 키워드
- 2018 FIGO staging system; Definitive radiotherapy; Diagnostic MRI; Nomogram; Uterine cervical cancer.
- 연구소개
- 2018년 개정된 자궁경부암의 FIGO 병기를 근치적 방사선치료를 받은 국소진행성 자궁경부암 환자 677명을 대상으로 검증한 논문입니다. 개정판의 권고대로 자기공명영상(MRI)으로 진단된 환자들을 대상으로 하여 새로 추가된 IIIC1/IIIC2 (골반/대동맥주위 림프절 전이) 병기에서 T 병기를 비롯한 국소 종양 인자들이 환자의 무진행 생존율(progression-free survival)을 결정하는 인자임을 보여주었고 노모그램을 통해 더 정확한 예후를 예측할 수 있었다는 점에서 부인종양학 연구자들에게 도움이 되는 논문이라고 생각합니다.
- 덧글달기
- 이전글 [Oral Oncol.] Clinical features of post-radiation nasopharyngeal necrosis and their outcomes following surgical intervention in nasopharyngeal cancer patients
- 다음글 [Radiol Med.] Clinical significance of radiation dose-volume parameters and functional status on the patient-reported quality of life changes after thoracic radiotherapy for lung cancer: a prospective study







