글로벌 연구동향
방사선종양학
- 2021년 01월호
[Radiother Oncol.] Heart substructural dosimetric parameters and risk of cardiac events after definitive chemoradiotherapy for stage III non-small cell lung cancer 폐암의 항암화학방사선치료에서 좌심실 방사선량과 심장부작용 위험도 분석서울의대 / 장범섭, 차명진, 장지현*
- 출처
- Radiother Oncol.
- 등재일
- 2020 Nov
- 저널이슈번호
- 152:126-132. doi: 10.1016/j.radonc.2020.09.050. Epub 2020 Oct 12.
- 내용
-
Abstract
Introduction: We evaluated the incidence of cardiac events after chemoradiotherapy in patients with stage III non-small cell lung cancer (NSCLC) based on baseline cardiovascular risk and the heart substructures' radiation dose.Methods: From 2008 to 2018, the cardiac events of 258 patients with stage III NSCLC who received definitive chemoradiotherapy were reviewed. The 10-year cardiovascular risk was calculated using the Atherosclerotic Cardiovascular Disease (ASCVD) scoring system. Dose-volume histograms were estimated for each cardiac chamber. A multivariate competing-risk regression analysis was conducted to assess each cardiac event's subhazard function (SHR).
Results: The median follow-up was 27.5 months overall and 38.9 months for survivors. Among the 179 deaths, none was definitely related to cardiac conditions. Altogether, 32 cardiovascular events affected 27 patients (10.5%) after chemoradiotherapy. Ten were major cardiac adverse events, including heart failure (N = 6) and acute coronary syndrome (ACS, N = 4). Most cardiovascular events were related to well-known risk factors. However, the volume percentage of the left ventricle (LV) receiving 60 Gy (LV V60) > 0 was significantly associated with ACS (SHR = 9.49, 95% CI = 1.28-70.53, P = 0.028). In patients with high cardiovascular risk (ASCVD score > 7.5%), LV V60 > 0% remained a negative ACS prognostic factor (P = 0.003). Meanwhile, in patients with low cardiovascular risk, the LV radiation dose was not associated with ACS events (P = 0.242).
Conclusions: A high LV radiation dose could increase ACS events in patients with stage III NSCLC and high cardiovascular risk. Pre-treatment cardiac risk evaluation and individualized surveillance may help prevent cardiac events after chemoradiotherapy.
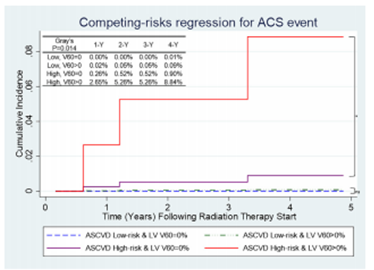
급성 관상동맥질환에 대하여 multivariate competing-risk regression analysis를 수행하였을 때, 낮은 ASCVD risk 의 환자에서는 LV V60 이 영향이 없었던 반면, 높은 ASCVD risk 에서는 (붉은선) 관련성이 높아짐을 보여주는 그래프입니다.
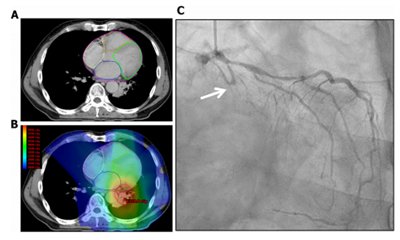
3기 비소세포폐암으로 진단받고 항암방사선치료를 받은지 6년이 경과되었을 때, 흉통으로 응급실에 내원한 환자의 관상동맥 조영술결과입니다 (C). 해당 검사에서 proximal left circumflex artery의 chronic total occlusion가 관찰되었으며, 해당 부위는 B에서 60 Gy 이상을 받은 부위와 일치하였습니다.
Affiliations
Bum-Sup Jang 1 , Myung-Jin Cha 2 , Hak Jae Kim 3 , Seil Oh 2 , Hong-Gyun Wu 3 , Eunji Kim 4 , Byoung Hyuck Kim 5 , Jae Sik Kim 6 , Ji Hyun Chang 7
1 Department of Radiation Oncology, Seoul National University Bundang Hospital, Seongnam-si, Republic of Korea.
2 Division of Cardiology, Department of Internal Medicine and Cardiovascular Center, Seoul National University Hospital, Republic of Korea.
3 Department of Radiation Oncology, Seoul National University College of Medicine, Republic of Korea.
4 Department of Radiation Oncology, Korea Institute of Radiological and Medical Sciences, Seoul, Republic of Korea.
5 Department of Radiation Oncology, SMG-SNU Boramae Medical Center, Seoul, Republic of Korea.
6 Department of Radiation Oncology, Seoul National University Hospital, Republic of Korea.
7 Department of Radiation Oncology, Seoul National University College of Medicine, Republic of Korea; Department of Radiation Oncology, Seoul National University Hospital, Republic of Korea. Electronic address: jh.chang@snu.ac.kr.
- 키워드
- Cardiac event; Chemoradiotherapy; Dosimetry; Heart substructure; Lung cancer.
- 연구소개
- 본 연구에서는 한국연구재단의 지원을 받아 258명의 비소세포폐암 환자에서 환자들의 baseline cardiovascular risk를 감안하여 방사선치료 시 심장의 세부구획에 대한 조사량이 이후 발생하는 심혈관계 event 에 얼마나 영향을 주는지를 분석하였습니다. 서울대학교병원 순환기내과 차명진 교수님과 함께 Atherosclerotic Cardiovascular Disease (ASCVD) scoring system을 이용하여 환자의 baseline cardiovascular risk를 자세히 평가하고자 하였고, 4개의 chamber를 따로 delineation 하여 각각의 dose-volume histogram parameter와 세분화된 주요 심혈관계 질환 사이의 관계를 multivariate competing-risk regression analysis를 이용하여 최대한 면밀하게 분석하고자 하였습니다. 분석 결과를 보면, 10.5%의 환자들에서 항암방사선치료 이후 심혈관계 이벤트가 있었지만, 대부분은 기존 가지고 있던 baseline cardiovascular risk factor 들과의 연관관계가 높았습니다. 방사선치료 관련한 parameter 중에서는, 좌심실에 60 Gy를 넘는 선량이 조사되었는지 여부 (LV V60 > 0%)가 이후의 급성 관상동맥질환과의 연관성을 보이는 것을 확인하였습니다. 이를 더욱 세분화하여 분석해보니, 기본적으로 baseline cardiovascular risk가 낮았던 환자들에게서는 LV V60 이 영향을 미치지 않았고, 기본 위험도가 높았던 환자들에게서만이 LV V60 이 의미를 갖는다는 것을 알게되었습니다. 결론적으로는, 기본적으로 높은 심혈관계 질환의 위험도를 가지고 있는 환자들에게서 심장, 특히 좌심실에 높은 방사선선량이 들어가야 하는 경우에는, 이후 individualized surveillance 가 필요하겠습니다.
- 덧글달기
- 이전글 [Sci Rep.] Efficacy and feasibility of proton beam radiotherapy using the simultaneous integrated boost technique for locally advanced pancreatic cancer
- 다음글 [Radiother Oncol.] Effect of baseline sarcopenia on adjuvant treatment for D2 dissected gastric cancer: Analysis of the ARTIST phase III trial







