글로벌 연구동향
방사선종양학
![[Clin Breast Cancer] Differences in Prognostic Factors and Failure Patterns Between Invasive Micropapillary Carcinoma and Carcinoma With Micropapillary Component Versus Invasive Ductal Carcinoma of th](/enewspaper/upimages/admin_20151110154927_R.jpg) 2015년 11월호
2015년 11월호
[Clin Breast Cancer] Differences in Prognostic Factors and Failure Patterns Between Invasive Micropapillary Carcinoma and Carcinoma With Micropapillary Component Versus Invasive Ductal Carcinoma of th성균관의대 / 최두호*
- 출처
- Clin Breast Cancer
- 등재일
- 2015 Oct
- 저널이슈번호
- 15(5):353-361.e2. doi: 10.1016/j.clbc.2015.01.008. Epub 2015 Feb 7.
- 내용
Author informationYu JI1, Choi DH2, Huh SJ1, Cho EY3, Kim K4, Chie EK4, Ha SW4, Park IA5, Ahn SJ6, Lee JS7, Shin KH8, Kwon Y8, Kim YB9, Suh CO9, Koo JS10, Kim JH11, Jeong BG12, Kim IA13, Lee JH14, Park W1.
1Department of Radiation Oncology, Samsung Medical Center, Sungkyunkwan University School of Medicine, Seoul, Korea.
2Department of Radiation Oncology, Samsung Medical Center, Sungkyunkwan University School of Medicine, Seoul, Korea. Electronic address: doho.choi@samsung.com.
3Department of Pathology, Samsung Medical Center, Sungkyunkwan University School of Medicine, Seoul, Korea.
4Department of Radiation Oncology, Seoul National University College of Medicine, Seoul, Korea.
5Department of Pathology, Seoul National University College of Medicine, Seoul, Korea.
6Department of Radiation Oncology, Chonnam National University Medical School, Gwangju, Korea.
7Department of Pathology, Chonnam National University Medical School, Gwangju, Korea.
8Center of Breast Cancer, National Cancer Center, Goyang, Korea.
9Department of Radiation Oncology, Yonsei University College of Medicine, Seoul, Korea.
10Department of Pathology, Yonsei University College of Medicine, Seoul, Korea.
11Department of Radiation Oncology, Dongsan Medical Center, Keimyung University School of Medicine, Daegu, Korea.
12Department of Radiation Oncology, Gyeongsang Institute of Health Sciences, Jinju, Korea.
13Department of Radiation Oncology, Seoul National University Bundang Hospital, Seongnam, Korea.
14Department of Radiation Oncology, St. Vincent's Hospital, The Catholic University of Korea College of Medicine, Suwon, Korea.
Abstract
PURPOSE:
We designed the present study to investigate differences in prognostic factors and failure patterns between patients with invasive micropapillary carcinoma or carcinoma with micropapillary component (IMPC) and randomly matched patients with invasive ductal carcinoma (IDC) of the breast at multiple institutions of the Korean Radiation Oncology Group (KROG).
MATERIALS AND METHODS:
This retrospective multicenter study was performed using subjects treated from January 1999 to November 2011. Female patients who had undergone curative resection for breast cancer without neoadjuvant chemotherapy were considered for this study. Exact matches were made for age (± 3 years), pathologic tumor and node stage, treatment method (surgery with or without radiotherapy), and period when surgery was performed (within 1 year) at the same institution.
RESULTS:
A total of 534 patients were analyzed. The median follow-up period was 59 months in both groups. In the comparison of clinicopathologic characteristics, rates of lymphovascular invasion (LVI) and nuclear grade III were both significantly higher in IMPC than in IDC (P < .001, P = .01, respectively). During the follow-up period, recurrences developed in 40 patients with IMPC (15.0%) and 21 with IDC (7.9%). Locoregional recurrence (LRR) developed in 22 patients with IMPC (8.2%) and 10 with IDC (3.7%). The rate of distant metastasis did not differ between the 2 groups (P = .52). LRR-free survival (P = .03) and recurrence-free survival (P = .007) were significantly different between the 2 groups, but overall survival was not (P = .67).
CONCLUSION:
IMPC is associated with a higher rate of LVI, high nuclear grade, and a propensity for LRR compared to IDC. Modification of the locoregional treatment modality might be needed in this pathologic subtype of breast cancer.
- 키워드
- Breast cancer; Case–control study; Invasive micropapillary carcinoma; Locoregional recurrence; Pattern of failure
- 연구소개
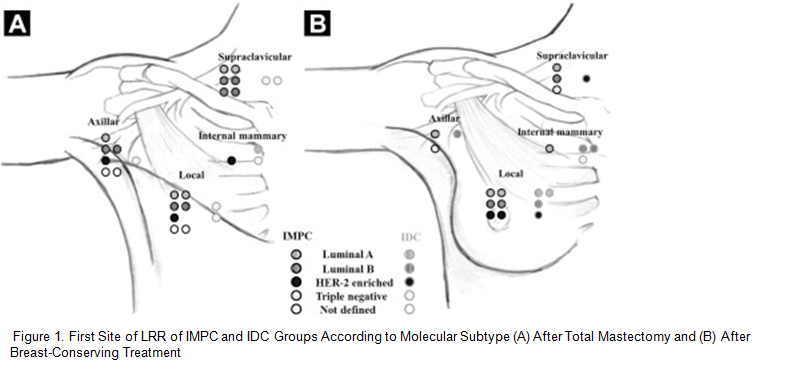
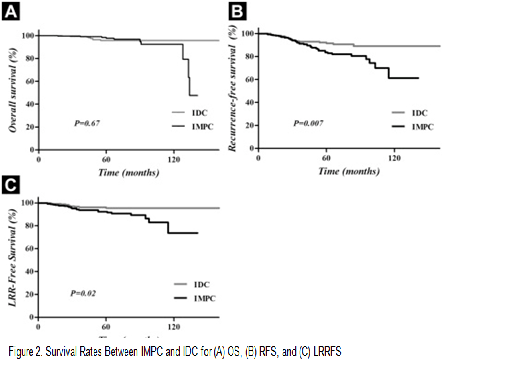
- Micropapillary carcinoma는 침윤성 유방암 중에서 비교적 최근에 병리학적으로 분류된 암으로 전체 유방암의 5% 정도의 비율을 차지 하며 림프혈관 침범이 빈번하고 림프절 전이를 잘하며 예후가 불량 할 수 있다는 점이 알려진 것 이외에 치료를 어떻게 이 질환에 맞추어 해야 할 것인가에 대한 연구가 별로 없었다. 특히 림프 관련 전이 가능성이 많아 원격 전이보다는 국소 재발이 더 잘 될 수 있다는 점에 유의하여 임상적으로 재발 형태를 보고 치료 방향을 제시 하고자 연구를 시행하였다. 본 연구자 들이 속해 있는 단일 기관에서의 선행 연구로 유방암에 대한 일반적인 치료 즉 수술, 항암 및 방사선치료, 그리고 필요 시 내분비 치료 후 재발 양상을 관찰한 결과 방사선치료 부위 안쪽 또는 부근에서 재발이 유방암에서 가장 흔한 type에 비해 많았음을 보고 하였으며 (breast 2010:19:231-7) 수술 후 병리학적 소견상 림프절 전이가 있는경우 다른 type보다 더 넓은 범위의 방사선치료가 필요하고 생각 하였고 좀 더 많은 환자를 대상으로 추가적으로 연구하기 위해 대한 방사선종양학회 다기관 연구 모임인 KROG에서 case-control study를 시행하였으며 선행 연구 결과를 더 확실하게 입증 하게 되었다. 그림 1에서 보듯이 유방절제술이나 유방보존술 이 후 추적 관찰한 모두 에서 micropapillary type이 방사선치료 범위 또는 근처의 부위에서 재발을 많이 하였으며 그림 2 에서 보듯이 무병 생존율이 낮았다. 수술 후 유방암에서의 방사선치료는 그 부위의 재발을 70% 이상 낮추는 것으로 잘 알려져 있으므로 이 type의 유방암은 임상적으로 방사선치료 시 좀 더 넒은 마진과 방사선량 등에서 더 적극적인 치료가 필요함을 제시 하고 있다. 이 논문의 아쉬운 점은 인용지수가 높은 저널 들에서 병리분야에서 central review를 하기를 요구하였으나 현실적으로 진행에 어려움이 있어서 인용지수가 높은 저널에는 채택이 안되었다는 점이지만 최근에 강조 되는 환자 맞춤형 치료의 관점에서 이 type의 환자는 방사선치료를 더 환자 맞춤형으로 적극적인 치료가 필요하다는데 의의가 있다.
- 덧글달기
- 이전글 [Radiother Oncol] Effects of adjuvant radiotherapy on completely resected gastric cancer: A radiation oncologist's view of the ARTIST randomized phase III trial.
- 다음글 [Radiother Oncol] High ratio of programmed cell death protein 1 (PD-1)(+)/CD8(+) tumor-infiltrating lymphocytes identifies a poor prognostic subset of extrahepatic bile duct cancer undergoing surgery







