글로벌 연구동향
방사선종양학
- 2019년 04월호
[Radiat Oncol.] Clinical predictors of radiation-induced lymphopenia in patients receiving chemoradiation for glioblastoma: clinical usefulness of intensity-modulated radiotherapy in the immuno-oncology era.교모세포종에서 방사선유발 림프구감소증의 예측인자 연구연세의대 / 변화경, 윤홍인*
- 출처
- Radiat Oncol.
- 등재일
- 2019 Mar 27
- 저널이슈번호
- 14(1):51. doi: 10.1186/s13014-019-1256-6.
- 내용
Abstract
BACKGROUND:
Immunotherapy is currently being examined as a treatment modality for glioblastoma. Maintaining an optimal total lymphocyte count (TLC) after radiotherapy (RT) and using temozolomide may be beneficial in optimizing immunotherapy. However, conventional temozolomide-based chemoradiation is known to induce immunosuppressive effects, including lymphopenia. Therefore, this study aimed to identify potential clinical predictors of acute severe lymphopenia (ASL) in patients receiving chemoradiation for glioblastoma.METHODS:
We identified patients with glioblastoma treated with RT plus temozolomide from 2006 to 2017. ASL was defined as a TLC of < 500/μL within 3 months after initiating RT. Independent predictors of ASL were determined using logistic regression.RESULTS:
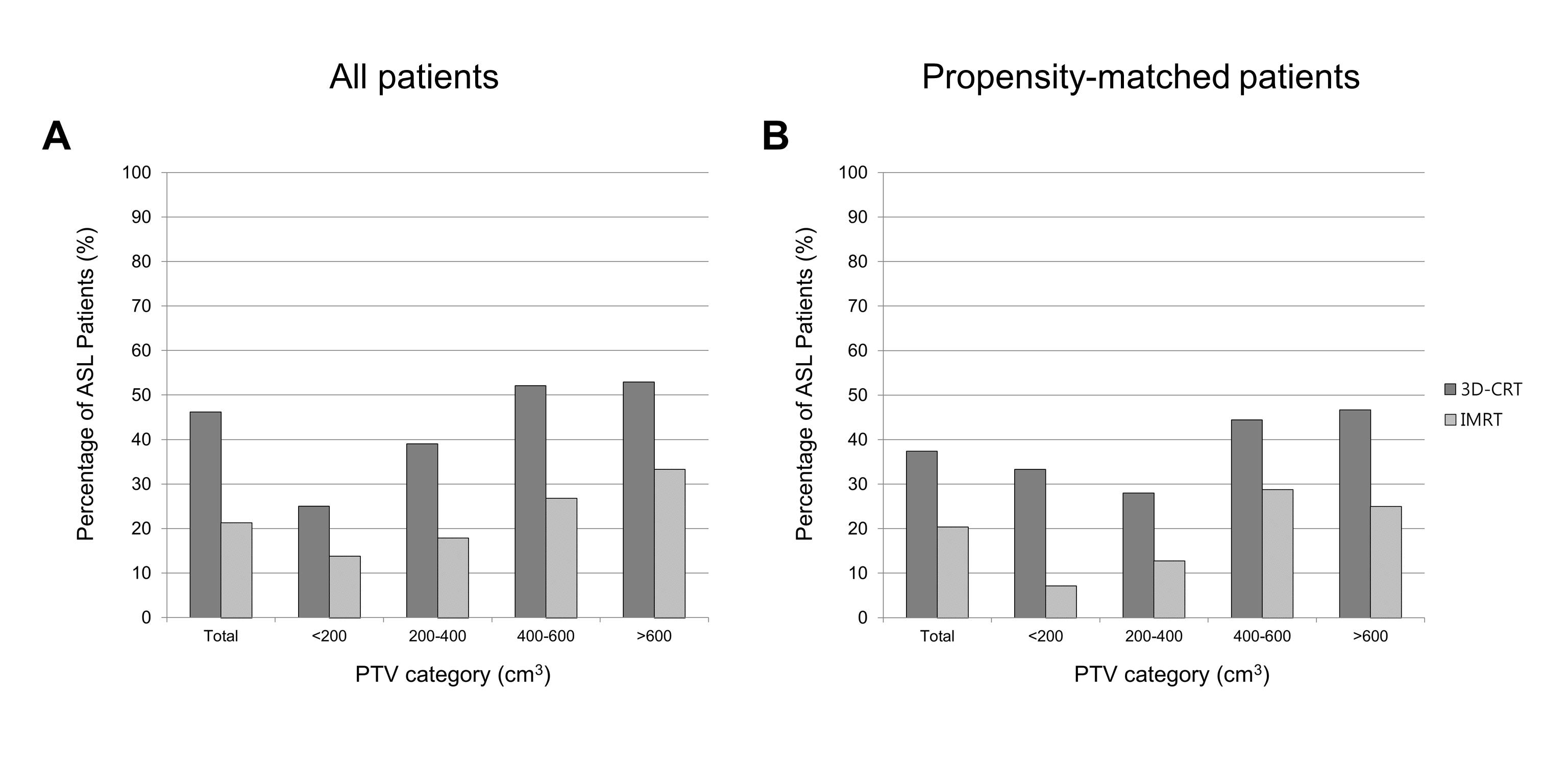
A total of 336 patients were evaluated. Three-dimensional conformal RT (3D-CRT) and intensity-modulated RT (IMRT) were used in 186 (55.4%) and 150 patients (44.6%), respectively. TLC decreased during RT and remained persistently low during the 1-year follow-up, whereas the levels of other blood cell types recovered. In total, 118 patients (35.1%) developed ASL. During a median follow-up of 19.3 months, patients with ASL showed significantly worse overall survival than did those without ASL (median, 18.2 vs. 22.0 months; P = .028). Multivariable analysis revealed that increased planning target volume (PTV) was independently associated with increased ASL incidence (hazard ratio [HR], 1.02; 95% confidence interval [CI], 1.00-1.03; P = .042), while IMRT was independently associated with decreased ASL incidence (HR, 0.48; 95% CI, 0.27-0.87; P = .015). A propensity-matched comparison showed that the incidence of ASL was lower with IMRT than with 3D-CRT (20% vs. 37%; P = .005).CONCLUSIONS:
IMRT and low PTV were significantly associated with decreased ASL incidence after RT plus temozolomide for glioblastoma. An IMRT-based strategy is necessary to enhance treatment outcomes in the immune-oncology era.
Author informationByun HK1, Kim N1, Yoon HI2, Kang SG3, Kim SH4, Cho J1, Baek JG1, Chang JH3, Suh CO1,5.
1
Department of Radiation Oncology, Yonsei Cancer Center, Yonsei University College of Medicine, 50-1 Yonsei-ro, Seodaemun-gu, Seoul, 03722, Republic of Korea.
2
Department of Radiation Oncology, Yonsei Cancer Center, Yonsei University College of Medicine, 50-1 Yonsei-ro, Seodaemun-gu, Seoul, 03722, Republic of Korea. YHI0225@yuhs.ac.
3
Department of Neurosurgery, Yonsei University College of Medicine, Seoul, Republic of Korea.
4
Department of Pathology, Yonsei University College of Medicine, Seoul, Republic of Korea.
5
Department of Radiation Oncology, CHA Bundang Medical Center, CHA University, Seongnam, Republic of Korea.
- 키워드
- Chemotherapy; Glioblastoma; Immunotherapy; Lymphopenia; Radiation; Treatment-related toxicity
- 연구소개
- 현재 면역항암제가 교모세포종을 비롯한 여러 암종에서 활발히 연구되고 있습니다. 임파구는 면역항암제의 작용에 중요한 역할을 합니다. 따라서 동시항암화학방사선요법으로 인해 발생하는 임파구 감소증을 줄일 방안이 필요합니다. 본 연구를 통해 교모세포종으로 동시항암화학방사선요법을 받은 336명을 후향적 분석하여 임파구 감소증에 영향을 미치는 인자를 밝혔습니다. 방사선치료 범위가 넓어질수록 임파구 감소증의 위험도가 높아지지만, 반대로 세기조절방사선치료를 사용했을 때에는 그 위험도가 효과적으로 낮아지는 결과를 보였습니다. 따라서 교모세포종의 방사선치료 시 세기조절방사선치료를 이용하는 것이 임파구 감소증에 도움이 되겠습니다. 또한 이는 장차 교모세포종에서 사용될 가능성이 있는 면역항암제의 작용을 증진시킬 수 있겠습니다.
- 덧글달기







