글로벌 연구동향
방사선종양학
![[Oncotarget.] Impact of radiation dose in postoperative radiotherapy after R1 resection for extrahepatic bile duct cancer: long term results from a single institution.](/enewspaper/upimages/admin_20170626164641_R.png) [Oncotarget.] Impact of radiation dose in postoperative radiotherapy after R1 resection for extrahepatic bile duct cancer: long term results from a single institution.
[Oncotarget.] Impact of radiation dose in postoperative radiotherapy after R1 resection for extrahepatic bile duct cancer: long term results from a single institution.서울의대 / 김병혁, 지의규*
- 출처
- Oncotarget.
- 등재일
- 2017 Apr 21.
- 저널이슈번호
- doi: 10.18632/oncotarget.17368. [Epub ahead of print]
- 내용
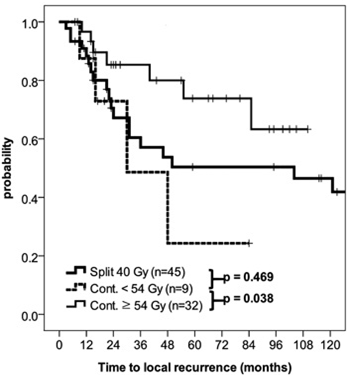
방사선량의 증량으로 국소제어율이 통계학적으로 유의하게 향상됨을 보여준 그림입니다. 아울러, 기존 방사선량군에서 분할 치료와 연속 치료간에 차이가 없음도 확인하였습니다.
Abstract
PURPOSE:
This study was conducted to evaluate the impact of radiation dose after margin involved resection in patients with extrahepatic bile duct cancer.
METHODS:
Among the 251 patients who underwent curative resection followed by adjuvant chemoradiotherapy, 86 patients had either invasive carcinoma (n = 63) or carcinoma in situ (n = 23) at the resected margin. Among them, 54 patients received conventional radiation dose (40-50.4 Gy) and 32 patients received escalated radiation dose (54-56 Gy).
RESULTS:
Escalated radiation dose was associated with improved locoregional control (5yr rate, 73.8% vs. 47.1%, p = 0.069), but not disease-free survival (5yr rate, 43.4% vs. 32.6%, p = 0.490) and overall survival (5yr rate, 40.6% vs. 29.6%, p = 0.348). In multivariate analysis for locoregional control, invasive carcinoma at the margin (HR 2.957, p = 0.032) and escalated radiation dose (HR 0.394, p = 0.047) were independent prognostic factors. No additional gastrointestinal toxicity was observed in escalated dose group.
CONCLUSIONS:
Delivery of radiation dose ≥ 54 Gy was well tolerated and associated with improved locoregional control, but not with overall survival after margin involved resection. Further validation study is warranted.
Author information
Kim BH1,2, Chie EK1, Kim K3, Jang JY4, Kim SW4, Oh DY5, Bang YJ5, Ha SW1.
1Department of Radiation Oncology, Seoul National University College of Medicine, Seoul, Republic of Korea.2Division of Biological Warfare Preparedness and Response, Armed Forces Medical Research Institute, Daejeon, Republic of Korea.3Department of Radiation Oncology, Ewha Womans University School of Medicine, Seoul, Republic of Korea.4Department of Surgery, Seoul National University College of Medicine, Seoul, Republic of Korea.5Department of Internal Medicine, Seoul National University College of Medicine, Seoul, Republic of Korea.
이달의 방사선의학 연구자 인터뷰
- 키워드
- R1 resection; extrahepatic bile duct cancer; postoperative radiotherapy; radiation dose
- 연구소개
- 절연면 침윤이 동반된 간외담도암으로 수술 후 치료를 받은 환자를 대상으로 방사선량 증량을 시행한 단일 기관 후향적 분석 연구입니다. 다변량 분석에서 절연면에 침윤성 암종이 있는 경우와 방사선량을 증량한 경우가 국소제어율에 독립적인 예후 인자임을 확인하였습니다. 아울러, 방사선량 증량군에서의 단기 및 장기 부작용이 더 증가하지 않음도 확인하였습니다. 그러나, 방사선량 증량이 무병생존율이나 전체생존율의 향상으로 연결되지는 못하였습니다.
- 덧글달기
- 이전글 [Jpn J Clin Oncol.] Quality assurance for a multicenter Phase II study of stereotactic ablative radiotherapy for hepatocellular carcinoma ≤5 cm: a planning dummy run.
- 다음글 [HPB (Oxford).] Risk stratification and prognostic nomogram for post-recurrence overall survival in patients with recurrent extrahepatic cholangiocarcinoma.









