글로벌 연구동향
방사선종양학
- [Oncologist .] A Survey of Practice Patterns for Clinical Nodal Staging Prior to Neoadjuvant Chemotherapy in Breast Cancer
서울의대 / 이한별, 이경훈, 신경환*, 장지현*
- 출처
- Oncologist .
- 등재일
- 2023 Dec 11
- 저널이슈번호
- 28(12):e1142-e1151. doi: 10.1093/oncolo/oyad156.
- 내용
Abstract
Background: The importance of clinical staging in breast cancer has increased owing to the wide use of neoadjuvant systemic therapy (NST). This study aimed to investigate the current practice patterns regarding clinical nodal staging in breast cancer in real-world settings.Materials and methods: A web-based survey was administered to board-certified oncologists in Korea, including breast surgical, medical, and radiation oncologists, from January to April 2022. The survey included 19 general questions and 4 case-based questions.
Results: In total, 122 oncologists (45 radiation, 44 surgical, and 33 medical oncologists) completed the survey. Among them, 108 (88%) responded that clinical staging before NST was primarily performed by breast surgeons. All the respondents referred to imaging studies during nodal staging. Overall, 64 (52.5%) responders determined the stage strictly based on the radiology reports, whereas 58 (47.5%) made their own decision while noting radiology reports. Of those who made their own decisions, 88% referred to the number or size of the suspicious node. Of the 75 respondents involved in prescribing regimens for neoadjuvant chemotherapy, 58 (77.3%) responded that the reimbursement regulations in the selection of NST regimens affected nodal staging in clinical practice. In the case-based questions, high variability was observed among the clinicians in the same cases.
Conclusions: Diverse assessments by specialists owing to the lack of a clear, harmonized staging system for the clinical nodal staging of breast cancer can lead to diverse practice patterns. Thus, practical, harmonized, and objective methods for clinical nodal staging and for the outcomes of post-NST response are warranted for appropriate treatment decisions and accurate outcome evaluation.
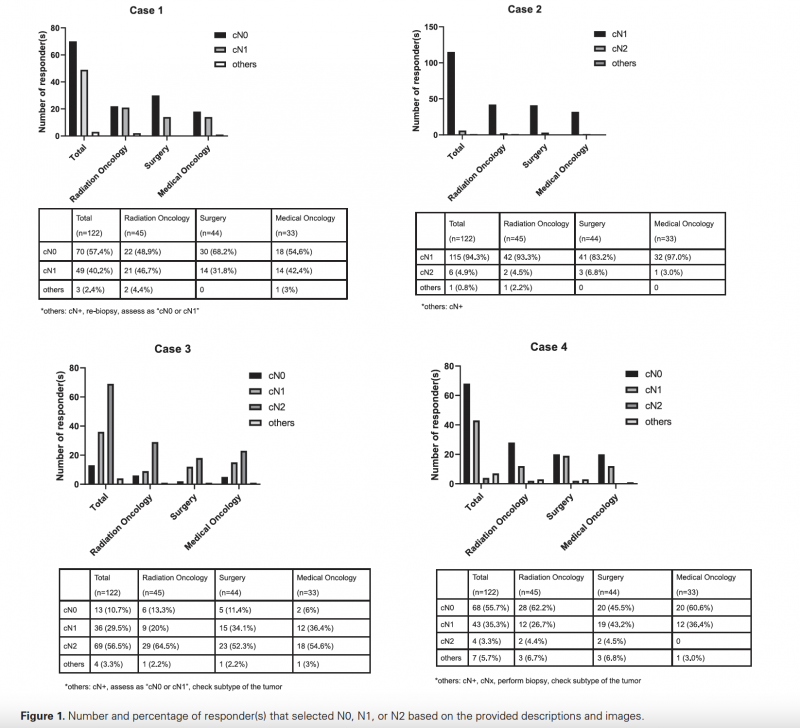
그림 설명: 같은 환자 case 에서도 각 과 별로 다양하게 nodal staging을 평가하는 양상을 보여주는 그래프.
Affiliations
Han-Byoel Lee 1 2 3, Kyung-Hun Lee 3 4 5, Seok Hyun Song 6, Kyubo Kim 7, Hong Kyu Kim 1 2 3, Hyeong-Gon Moon 1 2 3, Wonshik Han 1 2 3, Dae-Won Lee 4 5, Seock-Ah Im 3 4 5, Bum-Sup Jang 8 9, Yong Bae Kim 10, Jonghan Yu 11, Jee Hyun Kim 12, Yeon Hee Park 13, Kyung Hwan Shin 8 9, Ji Hyun Chang 8 9
1Department of Surgery, Seoul National University College of Medicine, Seoul, Republic of Korea.
2Biomedical Research Institute, Seoul National University Hospital, Seoul, Republic of Korea.
3Cancer Research Institute, Seoul National University, Seoul, Republic of Korea.
4Department of Internal Medicine, Seoul National University College of Medicine, Seoul, Republic of Korea.
5Department of Internal Medicine, Seoul National University Hospital, Seoul, Republic of Korea.
6Seoul National University College of Medicine, Seoul, Republic of Korea.
7Department of Radiation Oncology, Ewha Womans University College of Medicine, Seoul, Republic of Korea.
8Department of Radiation Oncology, Seoul National University College of Medicine, Seoul, Republic of Korea.
9Department of Radiation Oncology, Seoul National University Hospital, Seoul, Republic of Korea.
10Department of Radiation Oncology, Yonsei Cancer Center, Yonsei University College of Medicine, Seoul, Republic of Korea.
11Division of Breast, Department of Surgery, Samsung Medical Center, Sungkyunkwan University School of Medicine, Seoul, Republic of Korea.
12Department of Internal Medicine, Seoul National University Bundang Hospital, Seoul National University College of Medicine, Seongnam, Republic of Korea.
13Division of Hematology-Oncology, Department of Medicine, Samsung Medical Center, Sungkyunkwan University School of Medicine, Seoul, Republic of Korea.
- 키워드
- breast cancer; chemotherapy; neoadjuvant therapy; radiotherapy; staging; surgery.
- 연구소개
- 오랜 기간 동안 유방암의 치료는 수술 후 pathological staging을 기준으로 이후의 치료들을 결정하는 형태였습니다. 최근 유방암의 치료에서 선행항암화학요법의 사용이 확대되면서, pathological staging 뿐 아니라 clinical staging의 중요성도 증가하게 되었습니다. 그러나, 유방암에서 clinical 과 pathological nodal staging 의 기준이 상이하여 치료 방침을 정하기 어려운 경우가 많습니다. 이 연구는 국내 유방외과, 방사선종양학과, 혈액종양내과 전문의 122명에게 설문조사를 실시하여 실제 환경에서 유방암의 임상 림프절 병기에 대한 현재 진료 패턴을 조사했습니다. 연구 결과는 전문가들 사이에 같은 케이스에서도 실제로 다양한 평가가 이루어지고 있음을 보여주었으며, 이는 다양한 진료 패턴으로 이어졌습니다. 이 결과는 임상의들이 유방암의 nodal staging 에 대한 현재 상황을 인지하게 하였으며, 유방암의 진단, 치료 전략 및 적절한 결과 평가를 개선하기 위한 논의가 필요함을 시사하였습니다.
- 덧글달기
- 이전글 [Radiother Oncol .] Risk of on-treatment lymphopenia is associated with treatment outcome and efficacy of consolidation immunotherapy in patients with non-small cell lung cancer treated with concurrent chemoradiotherapy
- 다음글 [Int J Mol Sci .] Post-Radiotherapy Exosomal Non-Coding RNA and Hemograms for Early Death Prediction in Patients with Cervical Cancer










편집위원
유방암에서 선행항암화학요법의 시행이 증가하는 가운데, 임상적 N 병기에 대한 판단이 전공분야 및 개인에 따라 다양함을 보여주고, 이를 바탕으로 임상적 N 병기에 대한 객관적 기준의 필요성을 제시함
2024-02-05 16:38:37