글로벌 연구동향
방사선종양학
- [Front Oncol.] Adjuvant Radiotherapy Versus Surveillance for Grade 2 Intracranial Meningiomas: A Multi-Institutional Propensity Score-Matched Study 등급 II 뇌수막종에서 보조방사선치료의 다기관 성향점수매칭 분석
서울특별시보라매병원, 연세의대 / 변화경, 장원익, 위찬우*, 윤홍인*
- 출처
- Front Oncol.
- 등재일
- 2022 Jul 1
- 저널이슈번호
- 12:877244. doi: 10.3389/fonc.2022.877244. eCollection 2022.
- 내용
-
Abstract
Purpose: We aimed to compare the outcomes of adjuvant radiotherapy (ART) and surveillance in patients with grade 2 meningiomas (MNG2) who underwent surgical resection.Materials and methods: Data from four hospitals, in which patients aged ≥18 years underwent Simpson grade 1-4 surgical resection for newly diagnosed MNG2 between 1998 and 2018, were examined in this multicenter retrospective cohort study. Patients receiving ART with conventional fractionation were compared with those undergoing surveillance. Progression-free survival (PFS), progression/recurrence (P/R) were evaluated.
Results: This study included 518 patients, 158 of whom received ART. The median follow-up duration was 64.9 months. In the total cohort, ART was independently associated with significantly improved PFS (HR, 0.35; 95% CI, 0.23-0.55; P<0.001) and P/R (HR, 0.30; 95% CI, 0.18-0.48; P<0.001). In the propensity score-matched cohort (n=143 in each group), the 5-year PFS rates were 80.8% and 57.7% (P=0.004), and the 5-year P/R rates were 16.5% and 40.0% (P=0.002) in the ART and surveillance groups, respectively. After gross total resection, the 5-year PFS (85.0% vs. 64.7%; P=0.020) and P/R rates (15.2% vs. 32.0%; P=0.035) were significantly better in the ART group than in the surveillance group. A model for P/R was developed using recursive partitioning analysis with surgical extent, tumor size, and Ki-67 index. ART reduced the risk of P/R in the low- (P=0.069), intermediate- (P=0.044), and high-risk groups (P<0.001). Local control was also significantly enhanced by ART among all the risk groups (all P<0.05).
Conclusions: ART significantly improved PFS and P/R in patients with MNG2, irrespective of the surgical extent, and can be recommended after gross total resection. A prognostic model may guide decision-making for the use of ART.
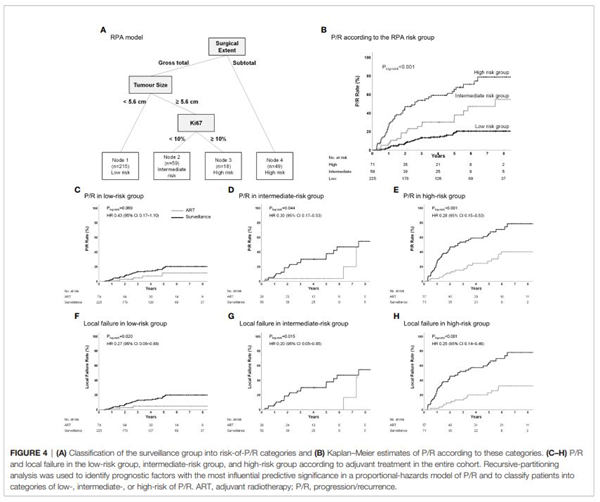
(A-B) 재발 위험도에 따라 환자군을 분류하였습니다.
(C-H) 모든 위험군에서 수술 후 방사선치료를 한 경우, 그렇지 않은 경우에 비해 재발률이 유의하게 감소하는 것으로 나타났습니다.
약어: ART, adjuvant radiotherapy; P/R, progression/recurrence.
Affiliations
Hwa Kyung Byun 1 , Won Ick Chang 2 , Joo Ho Lee 2 , Chul-Kee Park 3 , In Ah Kim 4 , Chae-Yong Kim 5 , Jaeho Cho 1 , Eui Hyun Kim 6 , Jong Hee Chang 6 , Seok-Gu Kang 6 , Ju Hyung Moon 6 , Sang Hyung Lee 7 , Jason Joon Bock Lee 8 , Il Han Kim 2 , Chang-Ok Suh 1 9 , Chan Woo Wee 10 11 , Hong In Yoon 1
1 Department of Radiation Oncology, Yonsei Cancer Center, Yonsei University College of Medicine, Seoul, South Korea.
2 Department of Radiation Oncology, Seoul National University Hospital, Seoul National University College of Medicine, Seoul, South Korea.
3 Department of Neurosurgery, Seoul National University Hospital, Seoul National University College of Medicine, Seoul, South Korea.
4 Department of Radiation Oncology, Seoul National University Bundang Hospital, Seoul National University College of Medicine, Seongnam, South Korea.
5 Department of Neurosurgery, Seoul National University Bundang Hospital, Seoul National University College of Medicine, Seongnam, South Korea.
6 Department of Neurosurgery, Severance Hospital, Yonsei University College of Medicine, Seoul, South Korea.
7 Department of Neurosurgery, Seoul Metropolitan Government - Seoul National University (SMG-SNU) Boramae Medical Center, Seoul, South Korea.
8 Department of Radiation Oncology, Kangbuk Samsung Hospital, Sungkyunkwan University School of Medicine, Seoul, South Korea.
9 Department of Radiation Oncology, Bundang CHA Medical Center, CHA University, Seongnam, South Korea.
10 Department of Radiation Oncology, Seoul Metropolitan Government - Seoul National University (SMG-SNU) Boramae Medical Center, Seoul, South Korea.
11 Department of Radiation Oncology, Seoul National University College of Medicine, Seoul, South Korea.
- 키워드
- adjuvant radiotherapy; intracranial meningioma; propensity score matching; surgical resection; surveillance.
- 연구소개
- 2등급 뇌수막종에서 수술 후 방사선치료를 했을 때 재발률이 낮아지는 것을 보여준 다기관 후향적 연구입니다. 수술적으로 부분절제 뿐만 아니라 완전절제 되었을 때에도 수술 후 방사선치료의 이득이 있는 것으로 밝혀졌습니다.
- 덧글달기










편집위원2
본 연구는 다기관의 뇌수막종 환자 cohort를 활용한 meta분석으로 기관별 보조방사선 치료 방법에 대한 분석을 통해 표준화된 가이드라인을 제시하고자 하는 연구 결과임.
2022-09-05 14:35:04