글로벌 연구동향
방사선종양학
- [Radiother Oncol.] Lymphocyte dynamics during and after chemo-radiation correlate to dose and outcome in stage III NSCLC patients undergoing maintenance immunotherapy
연세의대,MGH /조연아, 김예진, Clemens Grassberger*, 윤홍인*, 김진성*
- 출처
- Radiother Oncol.
- 등재일
- 2022 Mar
- 저널이슈번호
- 168:1-7. doi: 10.1016/j.radonc.2022.01.007. Epub 2022 Jan 13.
- 내용
Abstract
Purpose: We investigated the dynamics of lymphocyte depletion and recovery during and after definitive concurrent chemoradiotherapy (CCRT), dose to which structures is correlated to them, and how they affect the prognosis of stage III non-small cell lung cancer (NSCLC) patients undergoing maintenance immunotherapy.Methods and materials: In this retrospective study, absolute lymphocyte counts (ALC) of 66 patients were obtained before, during, and after CCRT. Persistent lymphopenia was defined as ALC < 500/μL at 3 months after CCRT. The impact of regional dose on lymphocyte depletion and recovery was investigated using voxel-based analysis (VBA).
Results: Most patients (n = 65) experienced lymphopenia during CCRT: 39 patients (59.0%) had grade (G) 3+ lymphopenia. Fifty-nine patients (89.3%) recovered from treatment-related lymphopenia at 3 months after CCRT, whereas 7 (10.6%) showed persistent lymphopenia. Patient characteristics associated with persistent lymphopenia were older age and ALC before and during treatment. In multivariable Cox regression analysis, recovery from lymphopenia was identified as a significant prognostic factor for Progression Free Survival (HR 0.35, 95% CI 0.13-0.93, p = 0.034) and Overall Survival (HR 0.24, 95% CI 0.08-0.68, p = 0.007). Voxel-based analysis showed strong correlation of dose to the upper mediastinum with lymphopenia at the end of CCRT, but not at 3 months after CCRT.
Conclusion: Recovery from lymphopenia is strongly correlated to improved survival of patients undergoing CCRT and adjuvant immunotherapy, and is correlated to lymphocyte counts pre- and post-CCRT. VBA reveals high correlation of dose to large vessels to lymphopenia at the end of CCRT. Therefore, efforts should be made not only for preventing lymphocyte depletion during CCRT but also for helping lymphocyte recovery after CCRT.
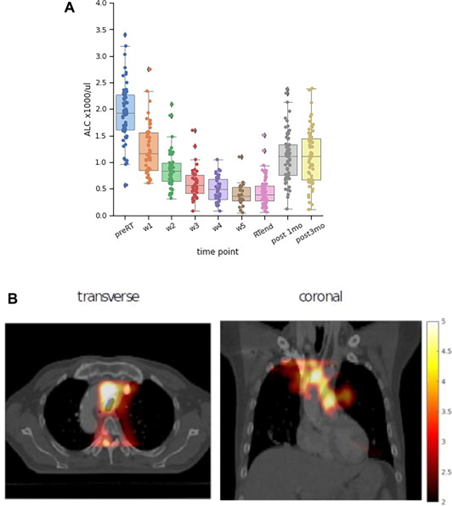
Fig. 2. A) The lymphocyte count before, during and after concurrent chemoradiotherapy(CCRT). B) Voxel-based analysis of the differences between patients with and without G3+ lymphopenia 3 months post-RT.
Affiliations
Yeona Cho 1 , Yejin Kim 2 , Ibrahim Chamseddine 3 , Won Hee Lee 4 , Hye Ryun Kim 5 , Ik Jae Lee 4 , Min Hee Hong 5 , Byung Chul Cho 5 , Chang Geol Lee 4 , Seungryong Cho 6 , Jin Sung Kim 7 , Hong In Yoon 8 , Clemens Grassberger 9
1 Department of Radiation Oncology, Gangnam Severance Hospital, Yonsei University College of Medicine, Yonsei University Health System, Seoul, Republic of Korea.
2 Department of Nuclear and Quantum Engineering, Korea Advanced Institute of Science and Technology, Daejeon, Republic of Korea; Department of Radiation Oncology, Massachusetts General Hospital and Harvard Medical School, Boston, United States; Department of Radiation Oncology, Yonsei Cancer Center, Yonsei University Health System, Yonsei University College of Medicine, Seoul, Republic of Korea.
3 Department of Radiation Oncology, Massachusetts General Hospital and Harvard Medical School, Boston, United States.
4 Department of Radiation Oncology, Yonsei Cancer Center, Yonsei University Health System, Yonsei University College of Medicine, Seoul, Republic of Korea.
5 Division of Medical Oncology, Department of Internal Medicine, Yonsei Cancer Center, Yonsei University College of Medicine, Seoul, Republic of Korea.
6 Department of Nuclear and Quantum Engineering, Korea Advanced Institute of Science and Technology, Daejeon, Republic of Korea.
7 Department of Radiation Oncology, Yonsei Cancer Center, Yonsei University Health System, Yonsei University College of Medicine, Seoul, Republic of Korea. Electronic address: JINSUNG@yuhs.ac.
8 Department of Radiation Oncology, Yonsei Cancer Center, Yonsei University Health System, Yonsei University College of Medicine, Seoul, Republic of Korea. Electronic address: yhi0225@yuhs.ac.
9 Department of Radiation Oncology, Massachusetts General Hospital and Harvard Medical School, Boston, United States. Electronic address: Grassberger.Clemens@mgh.harvard.edu.
- 키워드
- Absolute lymphocyte counts; Immune checkpoint inhibitor; Radiation-induced lymphopenia; Survival outcome; Voxel-based analysis.
- 연구소개
- 항암화학요법과 방사선치료를 동시에 받고, 이후에 면역치료를 받은 비소세포성 폐암 3기 환자군을 대상으로 혈액내 림프구 역동을 분석하고, 방사선치료가 림프구 감소증(lymphopenia)에 미치는 영향에 대하여 다면적으로 분석했습니다. 림프구 감소증은 방사선치료 후 발생할 수 있는 흔한 합병증 중 하나로, 최근 방사선치료와 면역치료의 병행효과가 각광받으며 그 중요성이 더욱 부각된 합병증입니다. 본 연구에서는 방사선화학치료 전/중/후의 림프구 역동을 분석하고, 이들이 환자의 생존율에 미치는 영향을 살펴보았습니다. 또한 방사선이 전달된 인체 부위 중 림프구 감소증과 그 상관관계가 높은 부위를 찾아냈습니다. 연구 결과 방사선화학치료 후 3개월 이내에 림프구 감소증에서 회복하는지 여부가 환자의 생존과 관련이 높음을 발견하였고, 이 회복 여부는 방사선 전/중의 림프구수와 상관관계가 높았습니다. 또한 거대혈관이 지나가는 상부 종격동(upper mediastinum)에 전달된 방사선이 치료직후 림프구 감소증 발생 여부와 높은 상관관계를 보였습니다. 따라서 본 연구자들은 더 나은 환자 생존율을 위해 해당 환자군들의 치료중 림프구수를 유지하기위한 노력을 기울어야 하며, 방사선치료계획에서 심장 뿐만 아니라 거대 혈관을 가지고 있는 상부 종격을 피하는 치료 전략이 필요함을 제안합니다.
- 덧글달기
- 이전글 [Radiat Oncol.] Optimal management of recurrent and metastatic upper tract urothelial carcinoma: Implications of intensity modulated radiation therapy
- 다음글 [Pediatr Blood Cancer.] Neurocognitive and psychological functioning of pediatric brain tumor patients undergoing proton beam therapy for three different tumor types









