글로벌 연구동향
방사선종양학
- [Ann Surg.] Risk of Lymphedema Following Contemporary Treatment for Breast Cancer: An Analysis of 7617 Consecutive Patients From a Multidisciplinary Perspective
연세의대 / 변화경, 장지석, 김용배*
- 출처
- Ann Surg.
- 등재일
- 2021 Jul 1
- 저널이슈번호
- 274(1):170-178. doi: 10.1097/SLA.0000000000003491.
- 내용
Abstract
Objective: The aim of this study was to identify the comprehensive risk factors for lymphedema, thereby enabling a more informed multidisciplinary treatment decision-making.Summary background data: Lymphedema is a serious long-term complication in breast cancer patients post-surgery; however, the influence of multimodal therapy on its occurrence remains unclear.
Methods: We retrospectively collected treatment-related data from 5549 breast cancer patients who underwent surgery between 2007 and 2015 at our institution. Individual radiotherapy plans were reviewed for regional nodal irradiation (RNI) field design and fractionation type. We identified lymphedema risk factors and used them to construct nomograms to predict individual risk of lymphedema. Nomograms were validated internally using 100 bootstrap samples and externally using 2 separate datasets of 1877 Asian and 191 Western patients.
Results: Six hundred thirty-nine patients developed lymphedema during a median follow-up of 60 months. The 3-year lymphedema incidence was 10.5%; this rate increased with larger irradiation volumes (no RNI vs RNI excluding axilla I-II vs RNI including axilla I-II: 5.7% vs 16.8% vs 24.1%) and when using conventional fractionation instead of hypofractionation (13.5% vs 6.8%). On multivariate analysis, higher body mass index, larger number of dissected nodes, taxane-based regimen, total mastectomy, larger irradiation field, and conventional fractionation were strongly associated with lymphedema (all P < 0.001). Nomograms constructed based on these variables showed good calibration and discrimination internally (concordance index: 0.774) and externally (0.832 for Asian and 0.820 for Western patients).
Conclusions: Trimodality breast cancer treatment factors interact to promote lymphedema. Lymphedema risk can be decreased by deintensifying node dissection, chemotherapy regimen, and field and dose of radiotherapy. Deescalation strategies on a multidisciplinary basis might minimize lymphedema risk.
Affiliations
Hwa Kyung Byun 1 , Jee Suk Chang 1 , Sang Hee Im 2 , Youlia M Kirova 3 4 , Alexandre Arsene-Henry 3 , Seo Hee Choi 1 , Young Up Cho 5 , Hyung Seok Park 5 , Jee Ye Kim 5 , Chang-Ok Suh 1 6 , Ki Chang Keum 1 , Joo Hyuk Sohn 7 , Gun Min Kim 7 , Ik Jae Lee 8 , Jun Won Kim 8 , Yong Bae Kim 1
1 Department of Radiation Oncology, Yonsei Cancer Center, Yonsei University College of Medicine, Seoul, Korea.
2 Department of Rehabilitation Medicine, Severance Hospital, Yonsei University College of Medicine, Seoul, Korea.
3 Department of Radiation Oncology, Institut Curie, Paris, France.
4 University Versailles St Quentin, France.
5 Department of Surgery, Yonsei Cancer Center, Yonsei University College of Medicine, Seoul, Korea.
6 Department of Radiation Oncology, Bundang CHA Medical Center, CHA University, Gyeonggi-do, Korea.
7 Department of Internal Medicine, Yonsei Cancer Center, Yonsei University College of Medicine, Seoul, Korea.
8 Department of Radiation Oncology, Gangnam Severance Hospital, Yonsei University College of Medicine, Seoul, Korea.
- 연구소개
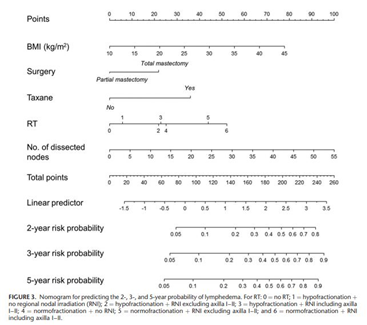
- 유방암 치료 후 발생하는 대표적인 부작용인 팔 림프부종에 관한 논문입니다. 그동안 림프부종 발생에는 겨드랑이 림프절 수술이 주로 관련한다고 생각되어왔습니다. 본 연구에서 대규모의 환자를 대상으로 분석한 결과 림프부종 발생에 여러가지 요인이 관련한다는 것이 밝혀졌습니다. 겨드랑이 림프절 절제 개수 뿐만 아니라 높은 체질량지수, 탁센계 항암제 사용, 넓은 방사선치료 범위, 높은 방사선치료 선량, 유방전절제술이 림프부종 발생과 연관이 있었습니다. 이렇게 밝혀진 요인들을 종합해서 개개인의 림프부종 발생 확률을 예측할 수 있도록 노모그램을 제작하였습니다. 본 노모그램을 통해서 유방암 환자의 치료 계획을 세울 때부터 림프부종의 위험성을 고려할 수 있으며, 림프부종 발생 고위험군을 선별하고 조기에 치료적 개입을 함으로써 유방암 환자들에게 도움이 될 수 있기를 바랍니다.
- 덧글달기










편집위원
유방암 방사선치료 후 림프부종의 위험인자를 5549명의 환자를 대상으로 후향적으로 분석한 논문으로, 통상분할조사가 소분할조사보다 림프부종의 위험도가 높다고 분석되었으며, 이 외의 다른 유의한 위험인자들을 이용하여 노모그램을 제시함.
2021-09-02 11:16:41