글로벌 연구동향
핵의학
- [Eur J Nucl Med Mol Imaging.] Preoperative [18F]FDG PET/CT tumour heterogeneity index in patients with uterine leiomyosarcoma: a multicentre retrospective study.
서울의대 / 이정원, 박정열, 정현훈*
- 출처
- Eur J Nucl Med Mol Imaging.
- 등재일
- 2018 Jul
- 저널이슈번호
- 45(8):1309-1316. doi: 10.1007/s00259-018-3975-6. Epub 2018 Feb 28.
- 내용
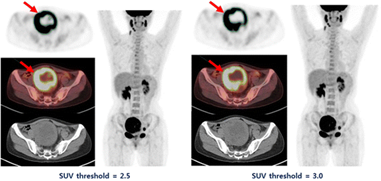
Fig. 1. SUV threshold 2.5와 3.0에서의 MTV 측정
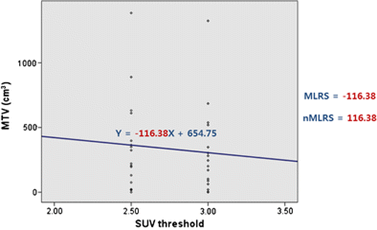
Fig. 2. MTV linear regression slope (MLRS)를 이용한 tumor heterogeneity 계산
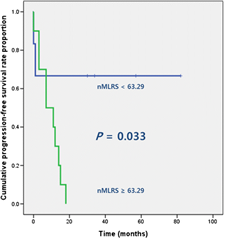
Fig. 3. Negative MLRS (nMLRS) 임계값으로 구분한 환자군의 무병생존 차이
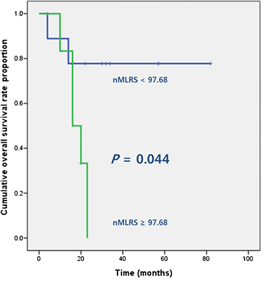
Fig. 4. Negative MLRS (nMLRS) 임계값으로 구분한 환자군의 전체생존 차이
Abstract
PURPOSE:
We investigated the prognostic value of the tumour heterogeneity index determined on preoperative [18F]FDG PET/CT in patients with uterine leiomyosarcoma (LMS).METHODS:
We retrospectively reviewed patients with uterine LMS who underwent preoperative [18F]FDG PET/CT scans at three tertiary referral hospitals. The PET/CT parameters maximum standardized uptake value of the primary tumour (SUVmax), metabolic tumour volume (MTV) and total lesion glycolysis were assessed. The negative values of the MTV linear regression slope (nMLRS) according to the SUV thresholds of 2.5 and 3.0 were determined as the tumour heterogeneity index. The value of PET/CT-derived parameters in predicting progression-free survival (PFS) and overall survival (OS) were determined in regression analyses.RESULTS:
Clinicopathological and PET/CT data from 16 patients were reviewed. The median postsurgical follow-up was 21 months (range 4-82 months), and 12 patients (75.0%) experienced recurrence. Tumour size (P = 0.017), SUVmax (P = 0.019), MTV (P = 0.016) and nMLRS (P = 0.008) were significant prognostic factors for recurrence. MTV (P = 0.048) and nMLRS (P = 0.045) were significant prognostic factors for patient survival. nMLRS was correlated with clinicopathological parameters including tumour size (Pearson's correlation coefficient γ = 0.825, P < 0.001) and lymph node metastasis (γ = 0.721, P = 0.004). Patient groups categorized according to the nMLRS cut-off value showed significant differences in PFS (P = 0.033) and OS (P = 0.044).CONCLUSION:
The preoperative tumour heterogeneity index obtained using the MTV linear regression slope may be a novel and useful prognostic marker in uterine LMS.
Author informationLee JW1, Park JY2, Lee HJ2, Lee JJ3, Moon SH4, Kang SY5, Cheon GJ5, Chung HH6.
1
Department of Obstetrics and Gynecology, Samsung Medical Center, Sungkyunkwan University School of Medicine, Seoul, Republic of Korea.
2
Department of Obstetrics and Gynecology, Asan Medical Center, University of Ulsan College of Medicine, Seoul, Republic of Korea.
3
Department of Nuclear Medicine, Asan Medical Center, University of Ulsan College of Medicine, Seoul, Republic of Korea.
4
Department of Nuclear Medicine, Samsung Medical Center, Sungkyunkwan University School of Medicine, Seoul, Republic of Korea.
5
Department of Nuclear Medicine, Cancer Research Institute, Seoul National University College of Medicine, Seoul, Republic of Korea.
6
Department of Obstetrics and Gynecology, Cancer Research Institute, Seoul National University College of Medicine, 101 Daehak-ro, Jongno-gu, Seoul, 03080, Republic of Korea. chhkmj@gmail.com.
- 키워드
- Linear regression; Tumour heterogeneity; Uterine leiomyosarcoma; [18F]FDG PET/CT
- 연구소개
- Uterine leiomyosarcoma 환자에서 수술 전 시행한 [18F]FDG PET/CT에서 측정한 tumor heterogeneity의 예후예측인자로써의 가치를 규명하고자 한 후향적 연구임. 3개의 3차 의료기관에서 수술 전 시행한 [18F]FDG PET/CT에서 SUV 2.5와 3.0에서 측정한 metabolic tumor volume(MTV)의 linear regression slope(MLRS)를 tumor heterogeneity index로 간주하였을 때의 무병생존과 전체생존과의 연관성을 규명하고자 하였음. 16명의 환자를 대상으로 한 분석에서, tumor size (P = 0.017), SUVmax (P = 0.019), MTV (P = 0.016), 그리고 MLRS (P = 0.008)가 무병생존의 유의한 예후인자였음. 또한, MTV (P = 0.048)와 MLRS (P = 0.045)가 전체생존의 유의한 예후인자였음. MRLS는 tumor size (Pearson’s correlation coefficient γ = 0.825, P < 0.001), lymph node metastasis (γ = 0.721, P = 0.004) 등 임상병리학적 예후인자와 연관성을 나타냄을 확인하였음. Uterine leiomyosarcoma 환자에서 수술 전 시행한 [18F]FDG PET/CT에서 계산한 MLRS는 새롭고 유용한 예후인자로 사용할 수 있음을 확인한 연구임.
- 덧글달기
- 이전글 [Ann Nucl Med.] Effects of rs591323 on serotonin transporter availability in healthy male subjects.
- 다음글 [Eur J Nucl Med Mol Imaging.] Dual-time point 18F-FDG PET/CT for the staging of oesophageal cancer: the best diagnostic performance by retention index for N-staging in non-calcified lymph nodes.









