글로벌 연구동향
방사선종양학
- 2021년 05월호
[Radiother Oncol.] Longitudinal impact of postmastectomy radiotherapy on arm lymphedema in patients with breast cancer: An analysis of serial changes in arm volume measured by infrared optoelectronic volumetry성균관의대 / 김나리, 김해영*, 황지혜*
- 출처
- Radiother Oncol.
- 등재일
- 2021 Mar 3
- 저널이슈번호
- 158:167-174. doi: 10.1016/j.radonc.2021.02.033. Online ahead of print
- 내용
Abstract
Background and purpose: This study was conducted to evaluate the longitudinal impact of postmastectomy radiation therapy (PMRT) on persistent severe lymphedema (PSL) using arm volume measurements by an infrared optoelectronic volumetry.Materials and methods: Of the patients who underwent mastectomy between 2008 and 2016, we included 330 patients with secondary arm lymphedema. Percentage of excessive volume (PEV) of the arm were serially assessed using an optoelectronic volumetry 1, 3, 6, 12, 18, 24, 36, and 48 months after the lymphedema diagnosis (Tlymh_Dx). We defined PSL as 2 or more episodes of PEV ≥ 20%. Risk factors for PSL were evaluated using stepwise regression analyses.
Results: Patients who received PMRT (n = 202, 61.2%) were more likely to have larger extent of axillary node dissection (AND), and frequent stage II/III lymphedema at Tlymh_Dx than those who did not receive PMRT (p < 0.001). With a median follow-up of 72.5 months, PSL occurred in 71 (21.5%) patients. Patients with PSL were more frequently treated with AND of ≥ 20 nodes without reconstruction, had advanced lymphedema stage and higher PEV at Tlymh_Dx, and more frequent events of cellulitis compared to those without PSL. The risk of developing PSL was significantly associated with PMRT with regional node irradiation (RNI), AND of ≥20 nodes, lymphedema stage, and PEV at Tlymh_Dx, cellulitis, and compliance with physical therapy.
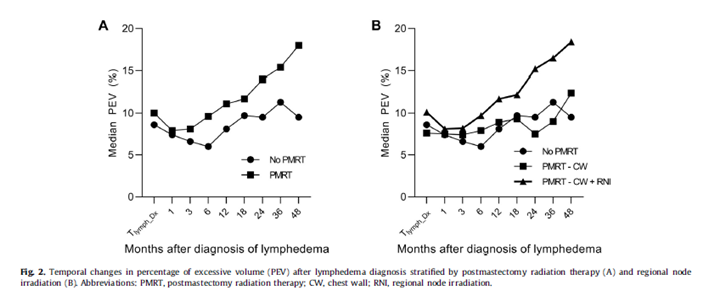
Conclusion: PMRT, especially RNI, was associated with a consistent increase in PEV in patients with arm lymphedema. Therefore, timely physical therapy is necessary for this patient population.
Affiliations
Nalee Kim 1 , Haeyoung Kim 2 , Ji Hye Hwang 3 , Won Park 1 , Won Kyung Cho 1 , Seung Mi Yeo 4 , Hyebin Lee 5 , Sei Kyung Lee 6
1 Department of Radiation Oncology, Samsung Medical Center, Sungkyunkwan University School of Medicine, Seoul, Republic of Korea.
2 Department of Radiation Oncology, Samsung Medical Center, Sungkyunkwan University School of Medicine, Seoul, Republic of Korea. Electronic address: haeyoung0131.kim@samsung.com.
3 Department of Physical & Rehabilitation Medicine, Samsung Medical Center, Sungkyunkwan University School of Medicine, Seoul, Republic of Korea. Electronic address: hwanglee@skku.edu.
4 Department of Physical & Rehabilitation Medicine, Samsung Medical Center, Sungkyunkwan University School of Medicine, Seoul, Republic of Korea.
5 Department of Radiation Oncology, Kangbook Samsung Hospital, Sungkyunkwan University School of Medicine, Seoul, Republic of Korea.
6 Department of Surgery, Samsung Medical Center, Sungkyunkwan University School of Medicine, Seoul, Republic of Korea.
- 키워드
- Breast cancer; Lymphedema; Mastectomy; Physical therapy; Radiation therapy.
- 덧글달기
- 이전글 [Korean J Intern Med.] Induction chemotherapy followed by concurrent chemoradiotherapy versus CCRT for locally advanced hypopharynx and base of tongue cancer
- 다음글 [Eur J Obstet Gynecol Reprod Biol.] Optimal treatment strategies for small cell carcinoma of the uterine cervix: A retrospective multi-center study (KROG 19-03)








편집위원
유방전절제술 및 방사선치료 후 발생하는 림프부종을 팔둘레가 아니라 체적으로 평가한 논문
덧글달기닫기2021-05-06 14:56:11
등록